When patients first hear the words “total joint replacement” applied to their jaw, the reaction is usually disbelief. Hips and knees, sure — but the jaw? It surprises people that the TMJ can be replaced at all, much less with custom-made titanium implants designed from a CT scan of their own anatomy. But for patients with severe, end-stage joint disease, total TMJ replacement is often the only option that actually solves the problem.
What is total TMJ replacement?
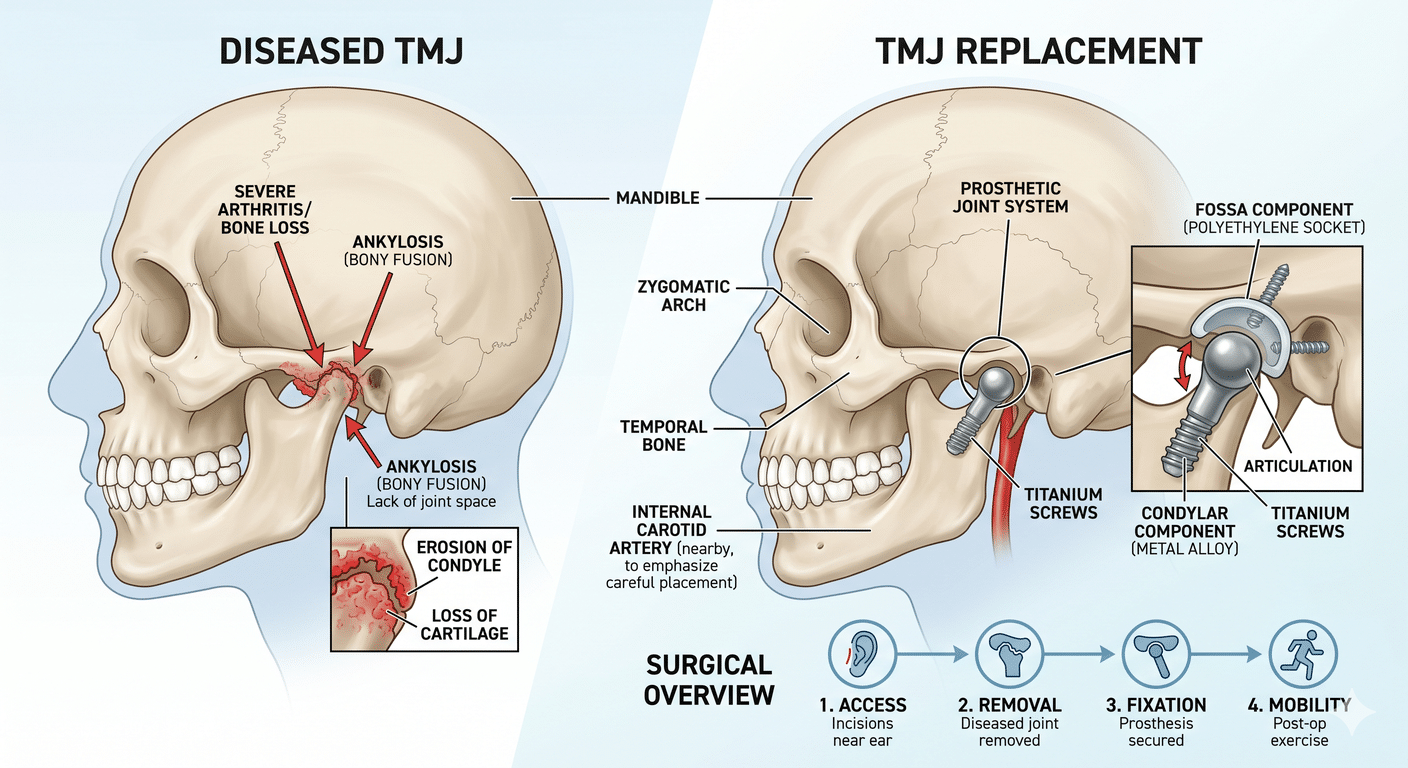
Total temporomandibular joint replacement is a surgical procedure that removes the diseased components of the jaw joint and replaces them with prosthetic parts. A complete prosthesis has two main components:
- A fossa component (the socket part) that attaches to the skull base
- A condylar component (the ball-and-ramus part) that attaches to the lower jaw
Modern systems used in this practice are made from medical-grade titanium with an ultra-high-molecular-weight polyethylene articulating surface. The implants used today are typically patient-specific, meaning they are custom-designed from a CT scan of the patient’s own bones to fit precisely against the existing anatomy.
Who actually needs a TMJ replacement?
Total joint replacement isn’t for jaw clicking or even for most TMJ pain. It’s reserved for patients whose joints are structurally destroyed or whose disease has not responded to other treatments. The most common indications are listed in detail in the end-stage TMJ pathology section, and they include:
- Severe osteoarthritis or rheumatoid arthritis with bone-on-bone changes
- Mandibular condylar resorption where the jaw bone is dissolving
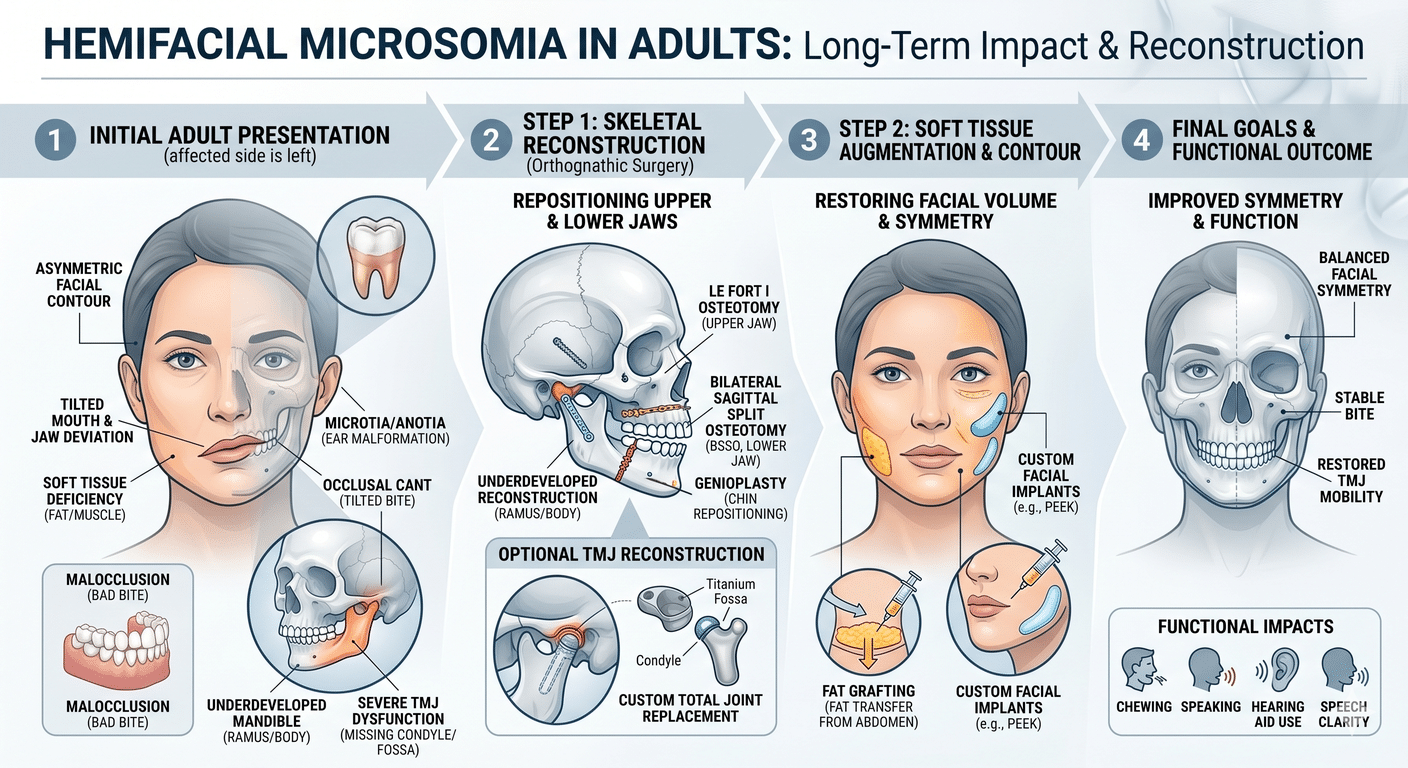
- Congenital absence or deformity of the joint such as in hemifacial microsomia
- TMJ ankylosis where the joint has fused and won’t move
- Failed prior joint surgeries, including failed Proplast/Teflon implants from the 1980s
- Severe joint trauma where the bone cannot be reconstructed
Many of these conditions overlap. A patient with an autoimmune condition like rheumatoid arthritis or lupus may have both severe joint destruction and a recessed jaw causing airway problems. In those cases, joint replacement is combined with orthognathic surgery in a single operation.
Why custom (patient-specific) implants matter
Stock implants — implants that come in a few generic sizes — were once the only option. They could be made to work, but they required the surgeon to shape the patient’s bone to fit the implant. Custom implants reverse that: the implant is designed to fit the patient.
Modern patient-specific TMJ prostheses offer real advantages:
- More precise fit, leading to better stability and longevity
- Less bone removal during surgery
- Predictable bite outcomes when combined with orthognathic surgery
- Built-in adjustments for facial asymmetry and existing deformity
- Shorter operating time once the implant is designed
The custom implant workflow is part of the broader virtual surgical treatment planning process used in this practice.
How is the surgery actually performed?
The procedure is done under general anesthesia and typically takes several hours, depending on whether orthognathic surgery is being performed at the same time. Incisions are placed in front of and below the ear, and the diseased joint components are removed. The fossa component is secured to the skull, the condylar component is attached to the lower jaw, and the bite and articulation are tested in the operating room before closing.
In a large number of cases, jaw advancement is performed simultaneously. Many TMJ replacement patients have airway compromise from years of joint disease pulling the lower jaw backward, and combining the two surgeries addresses both problems at once.
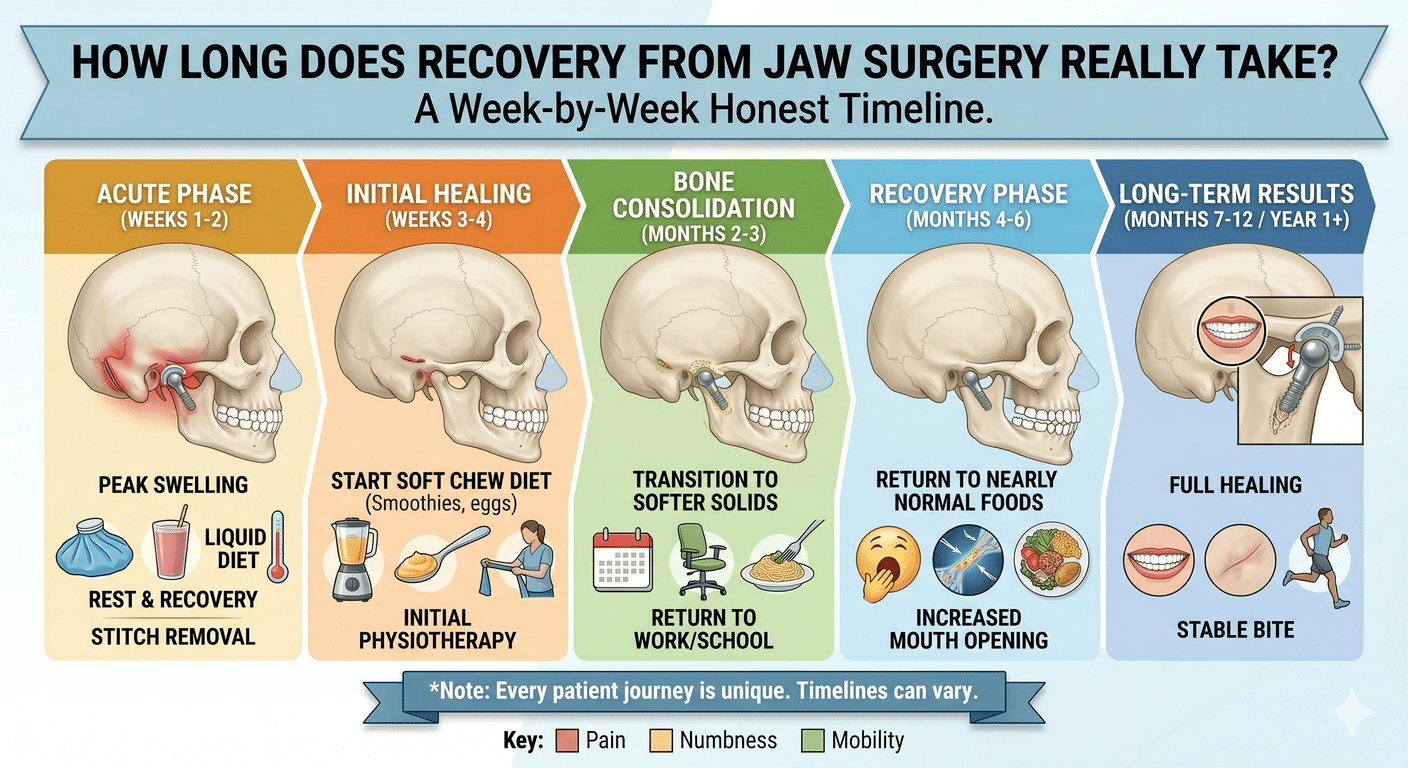
Recovering from total joint replacement takes more time than most jaw surgeries, but most patients are surprised by how manageable the pain is. Here’s a rough timeline of what recovery tends to look like:
- Days 1–3: You’ll be in the hospital on IV fluids and antibiotics while we keep swelling under control.
- First two weeks: Expect noticeable swelling. You’ll be on a soft or liquid diet, and we’ll start gentle physical therapy.
- Weeks 3–6: Most of the swelling goes down, and many patients are back at desk jobs by this point.
- Weeks 6–12: Physical therapy continues, and you’ll slowly work your way back to a normal diet.
- Months 3–12: Your bite, swelling, and jaw movement finish settling in. If any orthodontic touch-ups are needed, this is when they happen.
Physical therapy is critical and not optional. Patients who skip it tend to have inferior long-term opening. Detailed expectations are outlined on the postoperative instructions page.
How long do TMJ implants last?
Modern TMJ prostheses are designed to last decades, and many original recipients of current-generation devices have now had their implants in place for 20+ years without revision. The U.S. Food and Drug Administration tracks TMJ devices and the long-term performance data on contemporary systems is reassuring. That said, no joint replacement is permanent in the strict sense, and patients should expect routine long-term follow-up.
What about that history of failed TMJ implants?
Many patients have heard about the Proplast-Teflon TMJ implants used in the 1980s, which broke down in the body and caused severe damage. Those implants are not the same as today’s prostheses. Modern systems are made from biocompatible titanium and ultra-high-molecular-weight polyethylene — the same materials used in successful hip and knee replacements for decades.
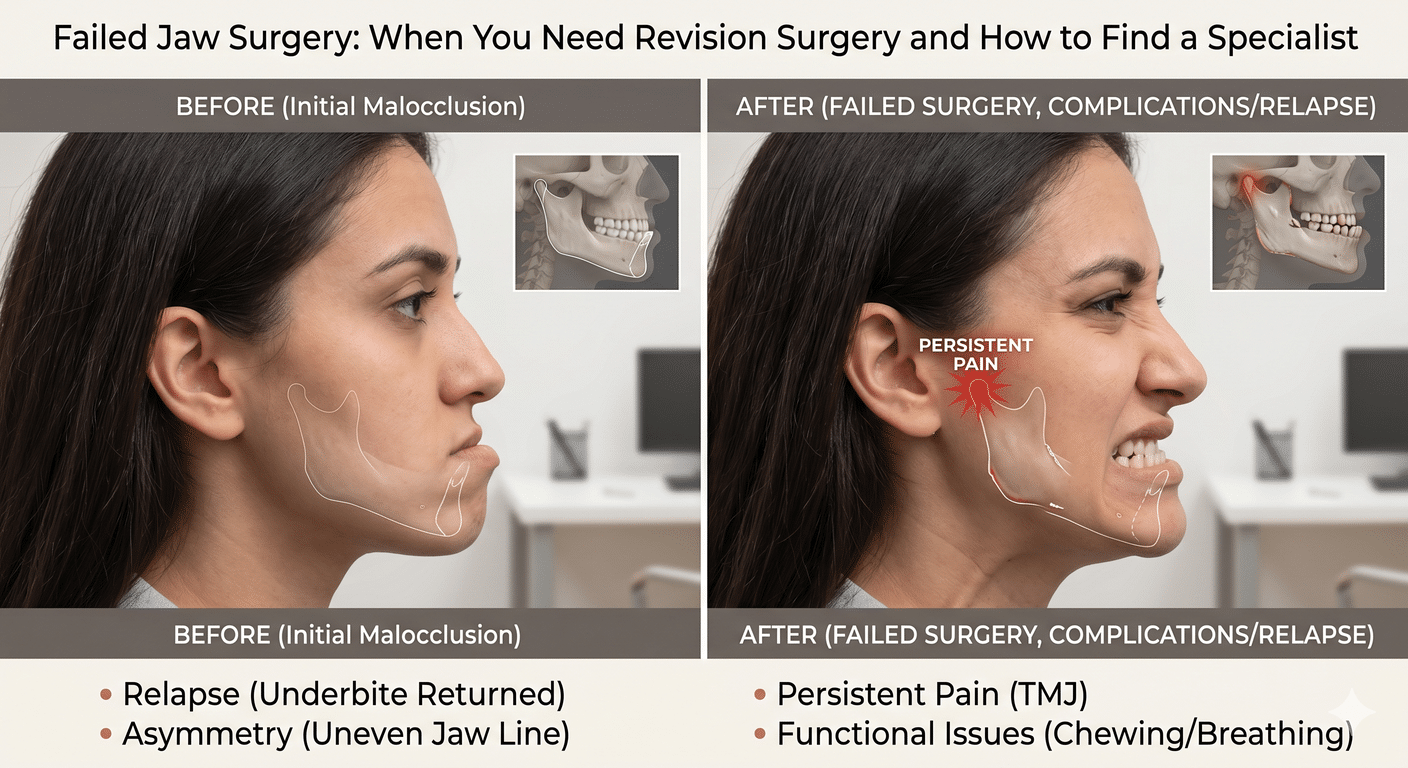
Patients who received older Proplast-Teflon or other failed implants are common candidates for complex revision surgery, which removes the failed device and replaces it with a modern custom prosthesis. Many of those revision cases are documented in the practice’s before-and-after gallery.
Outcomes patients can realistically expect
Realistic outcomes after total TMJ replacement include:
- Substantially reduced or eliminated joint pain
- Stable, predictable bite
- Improved opening (typically 30-40 mm or more)
- Improved chewing function and quality of life
- Often, improved facial balance and breathing if combined with jaw advancement
What patients should not expect: a jaw that moves exactly like a healthy native joint. The replacement joint hinges well but doesn’t slide forward and side-to-side the way a natural joint does. For most patients, this is a tradeoff they’re enthusiastic to make after years of severe pain and dysfunction.
The bottom line
Total TMJ replacement is one of the most life-changing operations in maxillofacial surgery. For patients with end-stage joint disease, no other treatment offers comparable, durable results. To learn more about whether you’re a candidate, schedule a consultation or call 214.828.9115 for a free 15-minute telephone consultation.