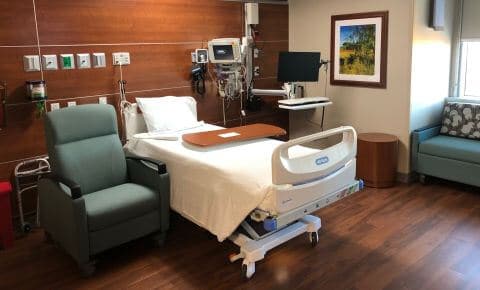
Hospital Stay
Please check our postoperative instructions for patient expectations and guidelines after oral and maxillofacial surgery with Dr. Wolford.
After surgery, you will awake in either the operating room or the recovery room. You will likely have a light pressure bandage around your jaws and over your head to support your jaws and reduce swelling. In addition, ice packs will be placed over your jaws and cheeks. With less involved surgery, you will be in the recovery room for a few hours before being moved to your private hospital room.
If surgery is performed on both the upper and lower jaws, you will likely stay in the recovery room overnight. Your family or friends can visit you there. While in the recovery room, you will have a nurse with you at all times in case you need anything. The next morning, you will be moved to your private hospital room where your family or friends can be with you 24 hours a day.
Typically, all of our patients go to Baylor Scott & White hospital after surgery. They get “16 Roberts”, the best floor of the entire hospital. They’re large private suites, and families can stay with the patient as well. The typical stay is 3-5 nights. Every room has a TV, fridge, and pull-out couch, with coffee and a microwave oven at the nurse station nearby. The insurance company pays for the hospital stay. Larry makes rounds twice a day, 365 days a year. After hospital discharge, we see patients for checkups for one year at no additional charge.
We use Gateway diagnostics for MRIs and CTs. They are 2 blocks north of Baylor hospital at 3310 Live Oak. If transportation is an issue, they will send an Uber to get you, FREE! Gateway is “in-network” with most insurance companies. Gateway also has Valium on hand for those patients who are anxious or claustrophobic.
In addition, your jaws will not be wired together and you will most likely be able to open and close your mouth immediately following surgery. Small rubber bands may be placed on the braces of your upper and lower teeth to help support your bite, minimize swelling in your TMJs, and decrease the stress on your jaw muscles. These elastics will also begin your post-surgical orthodontic treatment that will decrease your overall treatment time.
The First 24 Hours After The Surgery
Medications
Immediately post surgery, you will have a special button to push for self-administration of medication (PCA pump), to manage post-operative discomfort and pain. You will be switched to oral medication prior to leaving the hospital and for as long as needed afterward.
You will also be given:
- An antibiotic and usually a disinfectant mouth rinse to reduce the chances of infection
- A steroid to reduce swelling
- Ibuprofen or another NSAID to reduce inflammation and discomfort if needed
- Sudafed or a similar decongestant to reduce nasal congestion as needed
- Robitussin or a similar expectorant to thin secretions for easier swallowing if needed
- Anti-nausea medication as needed
Most patients can resume their regular medications the day after surgery, but be sure to confer with Dr. Wolford first.
Swelling
Facial swelling should be expected post surgery, but approximately 80% will be gone within 4 weeks. It typically takes several months before all swelling is gone. Ice packs are used immediately after surgery and can be help reduce swelling for the first 72 hours. After that time, the ice may not help reduce swelling, but many patients find the coolness feels good and continue to use the ice packs.
Diet
The first day after surgery you will begin drinking fluids and eating puree foods. (You will continue a puree diet following discharge and can usually progress to soft foods within 1 to 2 weeks.)
Avoid milk products, refined sugar and other sweets, and carbonated beverages for at least one week to decrease mucous production, help prevent decalcification of the teeth, and minimize bacteria media.
Your jaws will not be wired together making it easier for fluid and food intake. You will likely have light force elastics on your braces between your upper and lower teeth to maximize the fit of your teeth and keep you more comfortable initially post surgery. It is important to take in as much fluid as possible to prevent dehydration during this time. You can use a special feeding syringe (provided by the hospital), cup, glass, spoon or fork to get your fluids and food into your mouth. Do not use straws post operatively for the first 10 days, unless Dr. Wolford tells you otherwise.
Prior to hospital discharge, you must be able to drink fluids well, take in the puree meals, and take oral medications.
Oral Hygiene
Bring a child-size toothbrush and toothpaste with you to the hospital. Gentle brushing can begin the first day following surgery. Teeth should be brushed at least 3 times per day, and particularly after each meal.
A special mouthwash will be prescribed for you that will also help keep the teeth and gums clean.
A water-pick can be very helpful keeping the mouth clean, but can cause problems if used too early after surgery. Please check with Dr. Wolford before using a water-pick. Typically, water-picks are safe to use after 10 days on a low setting.
Miscellaneous Information
Your discharge day will likely be 1 to 4 days post surgery, but it will depend on the nature of the surgery and your individual response.
Do not blow your nose after surgery for 2 weeks, if upper jaw surgery was performed. It is OK to sniff backwards, but do not blow.
You may have a splint (like an orthodontic retainer) on the roof of your mouth after surgery to help stabilize your upper jaw and facilitate the healing process. Dr. Wolford will remove the splint at the appropriate time.
Most patients can take a lukewarm shower and wash their hair the second day after surgery, but be sure to check with Dr. Wolford before doing so. Do not take a hot shower, since this could make the patient light-headed.
Most sutures are self-resorbing, but some sutures may require removal around one week post surgery. Dr. Wolford uses special suturing techniques that allows for easy and painless removal.
Do not lift more than 20 pounds for at least one month following surgery. Please confer with Dr. Wolford as to when and how much you can lift after that time.
Returning to work will be dependent on the nature of your surgery, type of work that you do, and your post surgery progress. Some patients can return to work after 1 to 2 weeks, but others may require more time.
Orthodontic appliances will be required for a minimum of 4 to 6 months post surgery, but removal will be dependent on the orthodontist as when he feels the bite has reached maximum fit and function, which could extend treatment for a longer time. Orthodontic retainers will be required following completion of your orthodontic treatment.
Emergencies
If you have an emergency, call 911 immediately. Our office maintains a 24-hour answering system to provide the best possible medical care. Every attempt will be made to contact the patient or patient’s family as soon as possible to answer questions, refill medications, or aid in emergency care.
The First Week After The Surgery
Medications
It is important to take all medications as directed. Ibuprofen can be taken every 6 hours to help with pain and swelling. You may still need a stronger pain medication during the first week. Continue taking your antibiotic until the prescribed course is complete. If you have any questions about your medication, please contact our office.
Swelling
Swelling is typically most significant during the first week, but will begin to diminish shortly after. You can help swelling by keeping your head elevated above your heart level. Sleep in a recliner, elevate the mattress at the head, or use several pillows. Swelling of the nasal passages can be lessened by using a steam humidifier or by sitting in a steam shower. Be careful as shortly post surgery, heat can cause light-headedness and blackout.
Bleeding / Bruising
You should expect some minor bleeding from the surgical wounds and nasal passages during the first week, especially the first 72 hours after surgery. This is part of the healing process. However, in the rare occurrence of severe nasal bleeding, go immediately to the closest emergency room.
Bruising should resolve in about 3 weeks. You can expect bruising to change color and travel as it dissipates.
Facial Numbness
Facial numbness is also common and can last for weeks and sometimes months. Typically, numbness in the lower face and lips can last longer than numbness in the upper face.
Diet
You will need to continue a puree diet during the first week. You are not allowed to chew, but it is very important to stay hydrated. You should avoid alcohol and carbonated drinks during this time.
Oral hygiene
Continue using a baby sized, soft bristled toothbrush to clean the teeth, splint and adjacent gums (avoid the sutures and wounds). Also use a mouth rinse at least 2-3 times per day. Keeping your mouth as clean as possible will help prevent infection. You may also want to rinse with warm salt water to help soothe the wounds and promote faster healing.
Activity
You may return to very light work and activity during the first week. Activities like walking are encouraged, but do not overexert yourself. Each patient recovers at a different pace.
Follow-up
You will return for a post op appointment with Dr. Wolford during this first week to evaluate your healing and discuss any concerns.
The Second Week Postop
Swelling/Bruising
Both swelling and bruising will be significantly improved by the end of the second week. Bleeding should also have stopped by this time. You may experience some tingling as feeling begins to return to lips and face.
Diet
You can begin a soft food diet and will need to stay on soft foods for 3 – 4 months or as directed by Dr. Wolford. Continue to take in plenty of fluids and stay hydrated.
Oral hygiene
Continue good oral hygiene brushing and using mouth rinse 2-3 times a day and after meals.
Activity
You can ease back into regular activity as you see fit. However, exercise and strenuous activities should be avoided.
Third and Fourth Weeks Postop
Continue a soft food diet, and avoid any foods you have to chew. Light, non-impact exercise and activities are safe to resume. You should also be increasing your range of motion through jaw exercises. You should be ale to open your mouth moderately well by the end of the fourth week. If you are having significant difficulties, physical therapy may be indicated, but this is infrequently required.
Four to Six Weeks
You can return to the orthodontist and begin your final phase of orthodontic treatment. Ideally, either your orthodontist or Dr. Wolford should monitor and evaluate you every 1 to 2 weeks for the next 2 months, as your orthodontic teeth movements will occur more rapidly than before surgery.
Six Weeks and Beyond
You may have a follow up appointment with Dr. Wolford at 2 to 3 months post surgery. At this time you will discuss any further instructions and concerns. You will need to continue eating soft foods for 3 to 4 months post surgery. It takes approximately four months for the jawbones to adequately heal and withstand normal biting forces. The entire healing process will take approximately one year, but most patients are feeling pretty well at about 4 months post surgery.
If you have questions or would like to schedule an appointment, please contact Dr. Larry Wolford’s office using our online contact form or call 214-828-9115.