What is Mandibular Condylar Resorption?
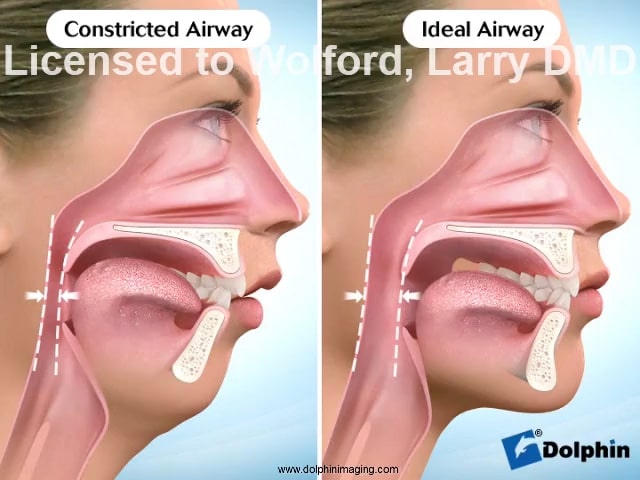
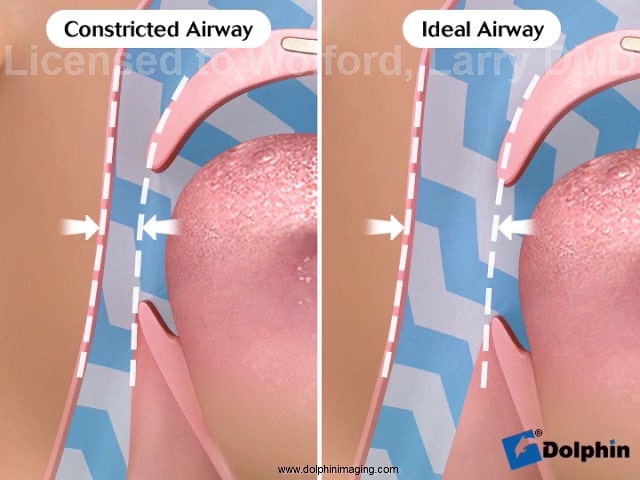
Mandibular condylar resorption is the breakdown and loss of bone in part of your temporomandibular joints (TMJs), or jaw joints. This bone loss affects the mandibular condyles, which are the rounded ends of your lower jaw that connect to your TMJ on both sides of your skull.
Condylar resorption causes your mandible, or lower jawbone, to shrink and retract (pull back). This change in your jaw may happen quickly (within months) or it can take years to develop.
Who Might Get Mandibular Condylar Resorption?
This condition is nine times more common in women than men. Condylar resorption usually affects women between 10 and 20 years of age.
How Does Mandibular Condylar Resorption Affect My Body?
It can cause changes to your facial appearance and structure. You may notice that your lower jaw looks smaller or your chin looks less defined.
Mandibular condylar resorption can also cause temporomandibular joint disorders (TMD). This inflammation in your muscles and ligaments around your jaw joints can lead to headaches, jaw pain and trouble moving your jaw.
Source: Cleveland Clinic
Mandibular Condylar Resorption Conditions
- Articular Disc Dislocation
- Adolescent Internal Condylar Resorption (AICR) Cases 3 And 4
- Reactive TMJ Arthritis Cases 5 And 6
- Mandibular Condylar Trauma
- TMJ Ankylosis Case 7
- Congenital Deformed/Absent TMJ (Hemifacial Microsomia) Case 8
- Connective Tissue And Autoimmune Diseases (CT/AI) Cases 9 And 10
- Other End-Stage TMJ Pathology
Articular Disc Dislocation
The most common TMJ pathology associated with dentofacial deformity is an anterior and/or medially displaced articular disc. This condition can initiate a cascade of events leading to arthritis and TMJ related symptoms.
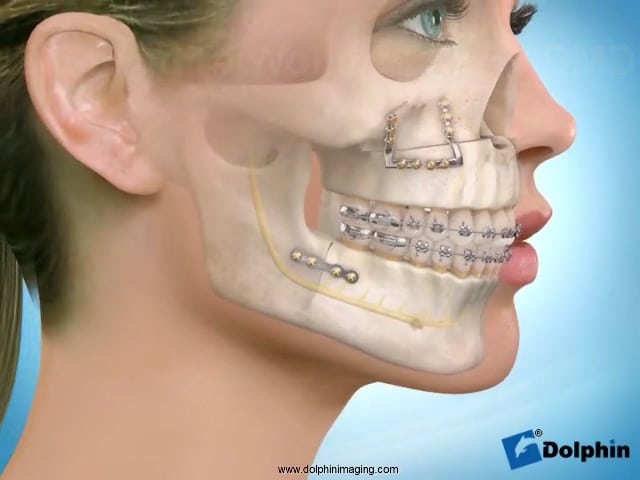
An MRI will show direction of disc displacement; progression of degeneration, mobility of joint components, etc. Simultaneous surgical treatment could include; reposition the TMJ disc into a normal anatomical, functional position and stabilize it using the Mitek anchor technique and required orthognathic surgical procedures to obtain optimal functional and esthetic outcomes.
For disc stabilization, two 0-Ethibond sutures (Ethicon Inc., Somerville, NJ) are threaded through the Mitek anchor islet and the anchor is placed into the posterior head of the condyle lateral to the mid-sagittal plane and approximately 8 mm below the crown of the condyle. The sutures are used as artificial ligaments to secure and stabilize the disc to the condylar head. The indicated orthognathic surgery is then performed at the same operation to correct the associated dentofacial deformity, or it can be delayed and performed at a secondary surgical stage.
In our studies using the criteria of incisal opening greater than 35 mm, stable skeletal and occlusal relationships, and significant reduction in pain, the success rate was 91%. The success rate was significantly better (95%) if the TMJ discs were surgically repositioned within the first 4 years of onset of the TMJ dysfunction without polyarthritic conditions. After 4 years, the progression of irreversible TMJ degenerative changes may result in a lower success rate. Significant degeneration of the TMJ may require total joint prostheses.
In patients with good facial balance, Class I occlusion, but with anteriorly displaced articular discs, repositioning the discs usually creates a malocclusion with end-on incisors relation and end-on Class III occlusion as well as posterior open bites. This occlusal change occurs because with displaced discs, the superior and posterior joint spaces decrease and the disc commonly thickens the longer it is displaced.
Therefore, when the disc is repositioned, the condyle is displaced downward and forward affecting the occlusal and skeletal relationship displacing the mandible toward an end-on Class III position. For patients who originally had a Class I occlusion, mandibular ramus sagittal split osteotomies may be required at the same operation to maintain the original occlusion and create space between the condyles and fossas to accommodate the repositioned discs.
Mandibular Condylar Videos