Hemifacial microsomia is one of the most common congenital craniofacial conditions, second only to cleft lip and palate. Children born with HFM have underdeveloped structures on one side of the face — most often the lower jaw, the temporomandibular joint, the cheekbone, the ear, and sometimes the soft tissues of the cheek. Most patients in the United States and similar healthcare systems receive at least some treatment in childhood. But many adults eventually realize that their childhood treatment, while helpful, wasn’t a finish line. The bite is off. The face is asymmetric. The joint is painful. Breathing at night is poor. The chin is recessed. The outcome is good — but not what they hoped for. The NIH Genetic and Rare Diseases Information Center has additional general background on hemifacial microsomia.
There is a great deal that can be done for hemifacial microsomia in adulthood — often more than patients realize.
What is hemifacial microsomia?
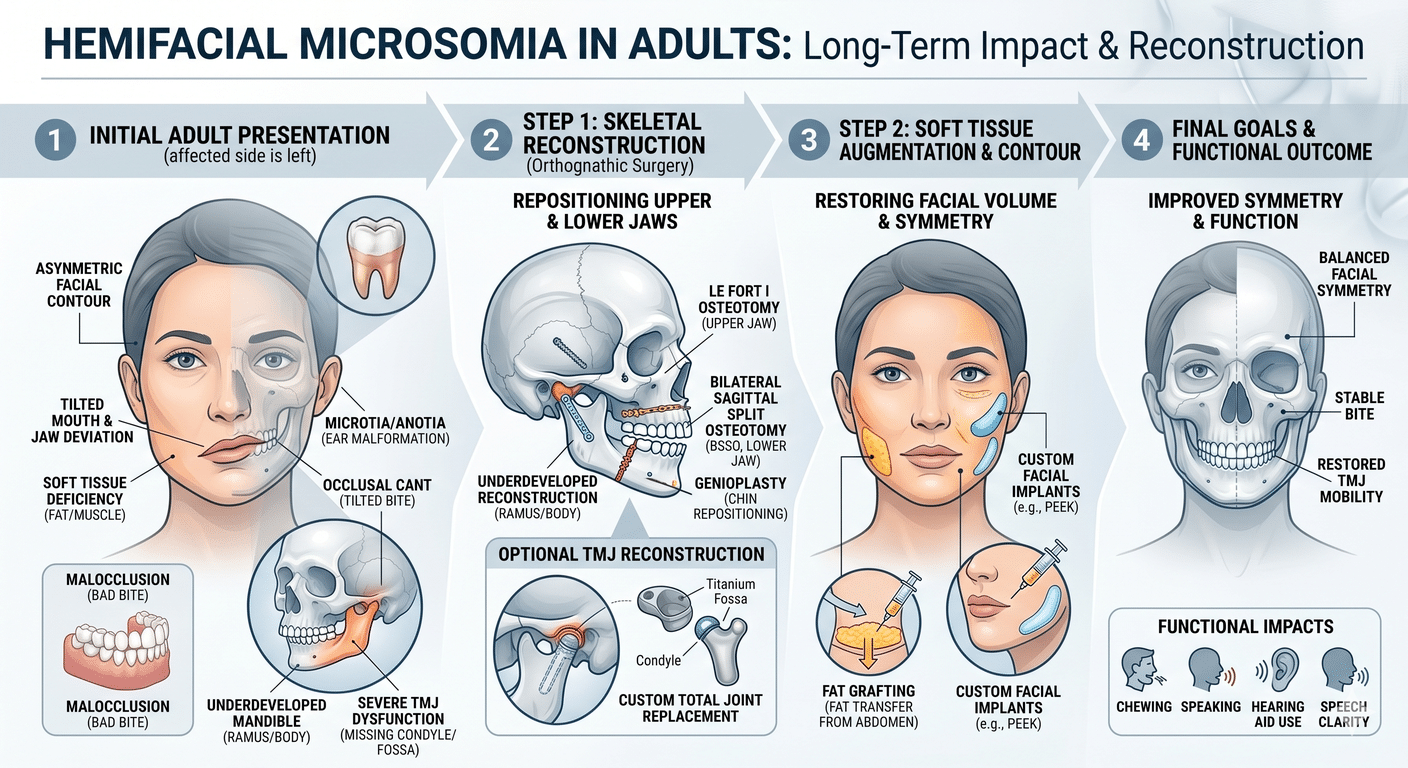
Hemifacial microsomia is a developmental condition that causes one side of the face to grow less than the other. The severity ranges widely. Some patients have mild asymmetry visible only to themselves; others have profound underdevelopment of an entire side of the face, including missing or grossly deformed jaw joint structures.
The typical structures affected include:
- The mandible (lower jaw), particularly the ramus and condyle
- The temporomandibular joint, sometimes entirely absent on the affected side
- The maxilla (upper jaw)
- The zygoma (cheekbone)
- The external ear
- Soft tissues, including the muscles of mastication and facial nerve branches
Because the condition affects bones that are still growing, treatment in childhood is staged over years. By the time a patient reaches adulthood, the goals shift. Childhood treatment focuses on growth and function. Adult treatment focuses on definitive correction. More background on related conditions is available on the broader craniofacial deformities page.
Why adult treatment is different (and often more effective)
Adult patients have a major advantage children don’t have: the bones are no longer growing. That changes everything about the surgical plan. In childhood, surgeons must aim for a moving target. In adulthood, the target is fixed, the planning can be precise, and the result can be definitive rather than provisional.
Modern adult HFM correction generally involves a combination of:
- Orthognathic surgery to bring both jaws into proper position and balance
- TMJ reconstruction or replacement where the joint is missing, deformed, or non-functional
- Bone grafting or augmentation to rebuild missing structures
- Genioplasty (chin surgery) to bring the chin into the midline and improve profile
- Soft tissue correction and, when indicated, fat grafting
- Airway-aware planning since OSA is common in this population
The TMJ piece — often the missing piece
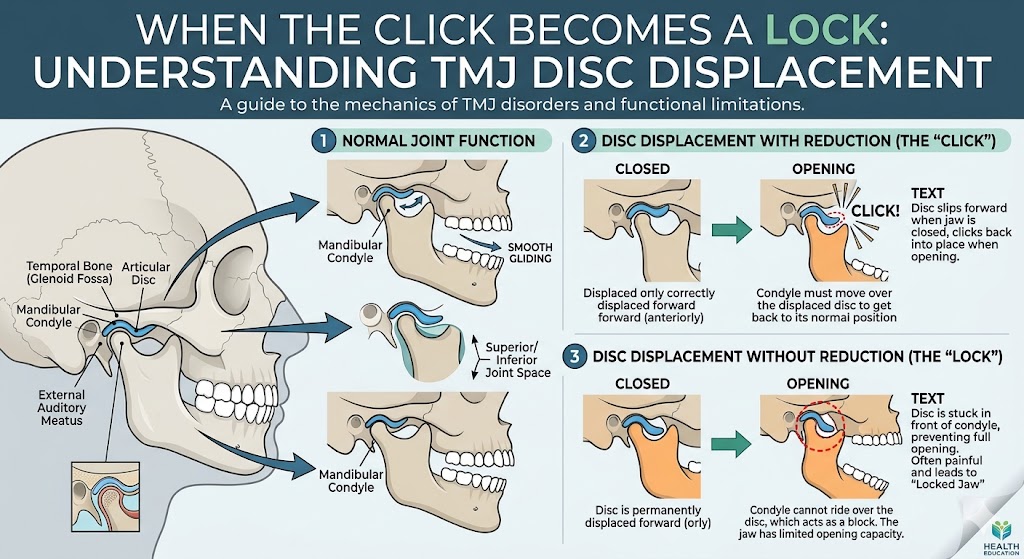
In many adult HFM patients, the affected TMJ is small, deformed, or completely absent. That hasn’t always been treated in childhood, and the consequences accumulate. Patients may have a deviated bite, severe asymmetry, limited opening, chronic pain, and progressive change as the abnormal joint quietly fails over decades. Patient-specific total TMJ replacement has dramatically changed what is achievable for these patients. Custom prostheses can be designed to match the missing anatomy, restore function, and serve as the foundation for simultaneous correction of the bite.
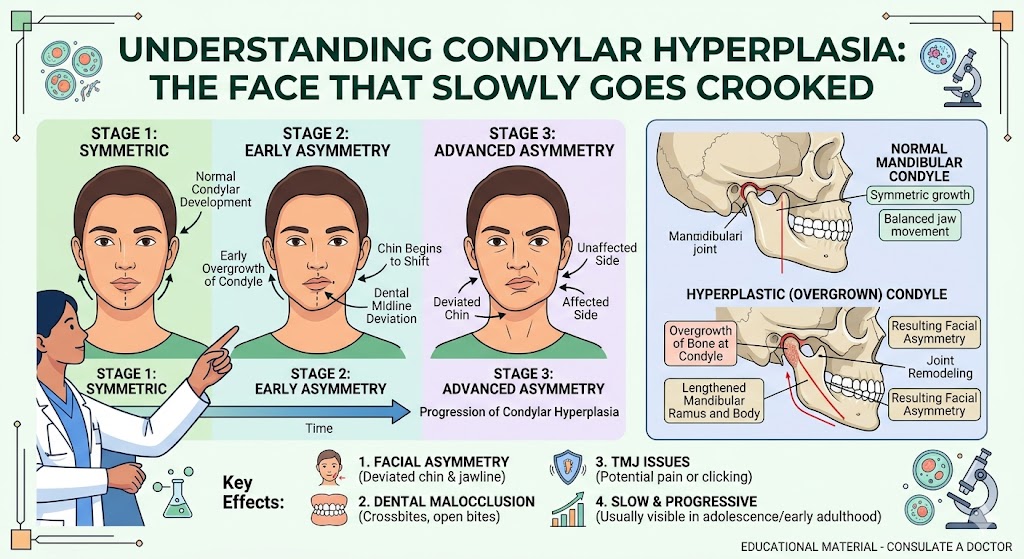
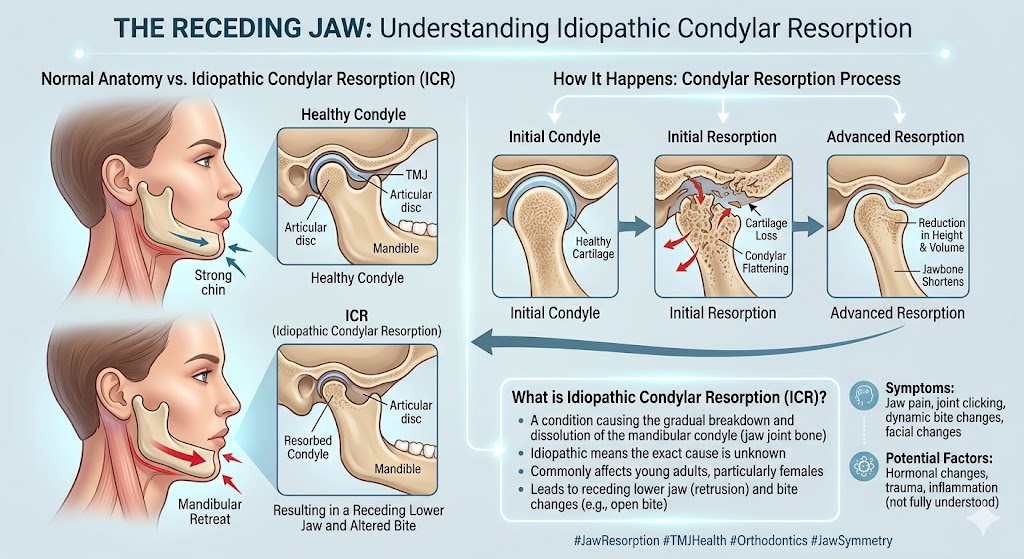
These cases overlap with the broader category of mandibular condylar resorption and reconstruction, since the surgical approach — custom joint replacement plus orthognathic surgery — is similar.
Airway and sleep apnea in adult HFM patients
Many adults with HFM have undiagnosed obstructive sleep apnea. When one side of the lower face is small, the airway behind the tongue is often narrow, and the lower jaw may be set back. Sleep apnea corrective surgery is therefore frequently combined with HFM reconstruction. Moving the jaws forward as part of the correction enlarges the airway at the same time it improves facial balance.
Patients are encouraged to complete the airway questionnaire for obstructive sleep apnea as part of their evaluation if any sleep symptoms are present.
How surgical planning works for these complex cases
Adult HFM correction is one of the most demanding categories of cases in maxillofacial surgery, and modern virtual surgical treatment planning is essential. CT scans are converted into 3D virtual models. The surgical plan is rehearsed digitally before it’s performed. Custom implants and surgical guides are designed and printed. By the time the patient is in the operating room, the operation has already been simulated.
This approach has been a quiet revolution for asymmetric and complex cases. Outcomes that were not realistically achievable 20 years ago are now routine.
What patients can realistically expect
Adult HFM correction generally produces:
- Significant improvement in facial symmetry
- Stable, functional bite
- Better breathing — both daytime and nighttime
- Reduction or elimination of TMJ pain
- Improved chewing and speech
- Restoration of facial balance
What it cannot do is make an asymmetric face perfectly symmetric. Realistic expectations are important — the goal is dramatic improvement, not perfection. Many patients describe the change in how the world responds to them as more meaningful than any single physical outcome.
Recovery and the road back
Recovery from combined HFM correction is similar to recovery from other major orthognathic and joint cases — covered in detail on the postoperative instructions page. Most patients return to work in two to four weeks, exercise in six to eight weeks, normal eating in six to eight weeks, and final results between six and twelve months.
For patients with cleft-related HFM features, the American Cleft Palate Craniofacial Association maintains general patient resources that complement surgical care.
The bottom line
Many adults with hemifacial microsomia were told, somewhere along the way, that there wasn’t much more to be done. That’s rarely true today. With modern joint replacement, virtual planning, and combined orthognathic-airway-joint surgery, dramatic improvement is possible — even decades after childhood treatment ended.
If you’ve grown up with hemifacial microsomia and are wondering whether more is possible, schedule a consultation or call 214.828.9115 for a free 15-minute telephone consultation. The travel information page is set up for patients coming from out of state and internationally, which describes a large portion of HFM patients seen in this practice.