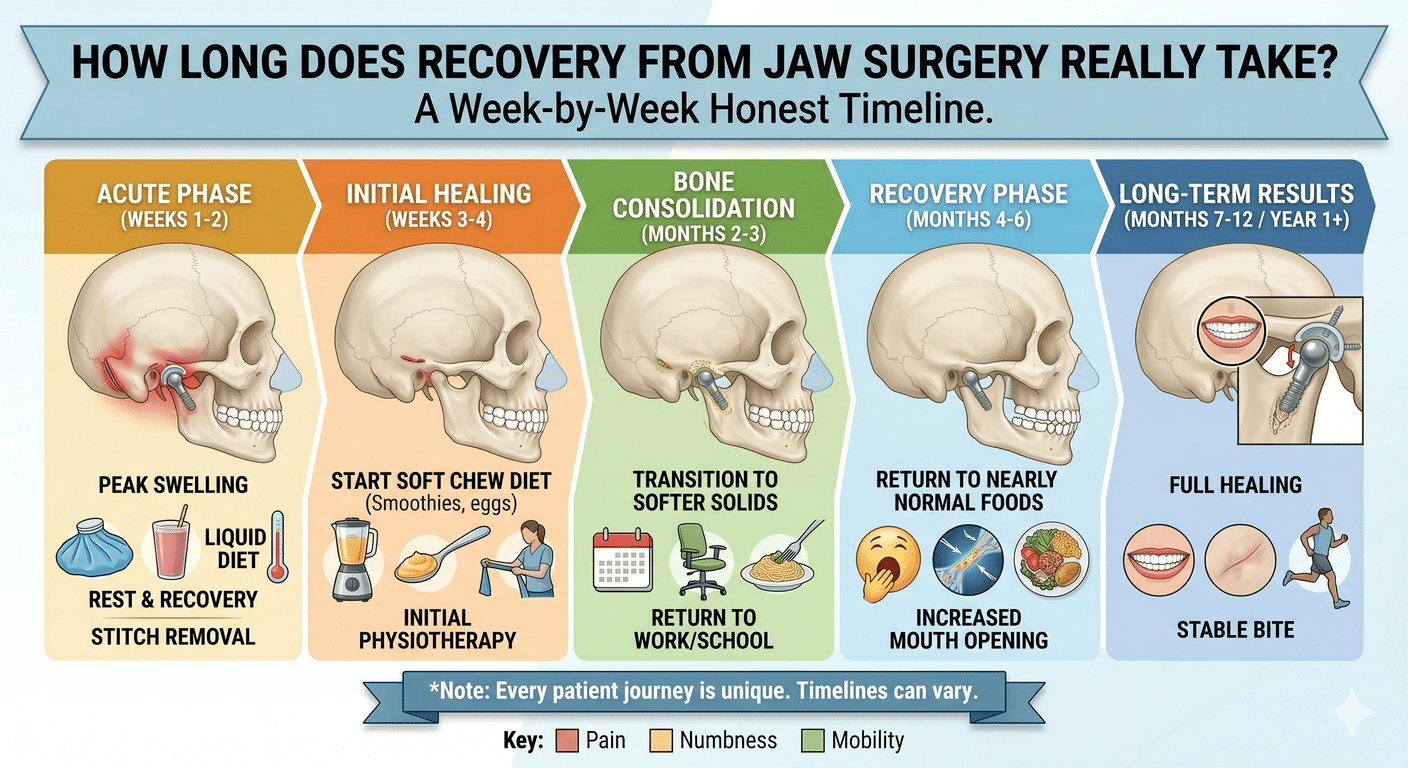
Jaw surgery recovery is the question patients ask more than any other, and online answers tend to fall into two categories: weirdly cheerful (“You’ll be fine in a week!”) or frightening (“It’s the worst pain of your life and you can’t eat for months”). Neither is accurate. Here is a realistic, week-by-week look at what recovery from orthognathic surgery actually looks like, drawn from thousands of patient experiences.
“Keep in mind this is a rough guide. Your actual recovery will depend on a lot — what kind of surgery you had (single jaw, double jaw, joint replacement), your age and overall health, whether you needed bone grafting, and how closely you stick to your surgeon’s instructions.”
Before surgery: the foundation
Recovery actually starts before the operation. Patients who arrive in good nutritional shape, with stopped tobacco/nicotine use, well-controlled medical conditions, and realistic expectations recover faster. Detailed prep guidance is available on the preoperative instructions page, and patients should also complete the appropriate patient medical information forms in advance.
Days 0-3: hospital and the first 72 hours
You’ll wake up swollen, congested, and cold from the operating room. Most patients spend one or two nights in the hospital. Pain is usually less intense than people fear — the bigger issue is pressure, swelling, and not being able to breathe through your nose easily. IV anti-inflammatories, ice, and head elevation are the foundation of comfort during this period.
By day three, most patients are home, sleeping propped up at about 45 degrees, taking medications by mouth, and managing a full-liquid diet.
Week 1: peak swelling, slow but steady
Swelling typically peaks around day three to five, then starts coming down. You’ll be on a full-liquid diet — protein shakes, blended soups, smoothies, broths. Brushing is gentle and limited at first. You’ll probably feel tired, slightly emotional, and frustrated with your face. All of that is normal.
Most patients are not on prescription opioid pain medication by the end of week one. Ibuprofen and acetaminophen, alternated, handle the discomfort for the majority of patients.
Week 2: the corner turns
Week two is usually when patients realize this is going to be okay. Swelling has dropped significantly. The puffiness shifts from “alien” to “recently had a procedure.” Numbness in the lower lip and chin is still present and will be for weeks to months — that’s normal and almost always resolves.
Many patients transition to a soft-no-chew diet around the end of week two. Think eggs, oatmeal, pasta, fish, soft cooked vegetables, and yogurt — anything that doesn’t require active chewing.
Weeks 3-4: back to the world
Most patients return to desk work and school somewhere between two and four weeks post-op. Energy starts to return. You can hold a normal conversation. Swelling is now subtle enough that strangers don’t notice. Light walking and gentle exercise are typically allowed; running and weights are not.
This is also when patients often need a small mental adjustment — your face is changing in real time, and even when the change is exactly what you wanted, it can feel strange in the mirror.
Weeks 5-8: chewing comes back
At six weeks post-op, patients typically advance to soft solids. Masticatory fatigue persists. Heavy lifting, contact sports, and high-impact activity remain restricted until week eight. Paresthesia continues to resolve. Splints, if placed, are adjusted or removed during this interval.
By week eight, the practical work of recovery is largely behind you. You’re eating, working, exercising, and looking like yourself.
Months 3-6: the cosmetic finish
Healing on the inside is still happening, even if the outside looks normal. Bone consolidates over six months. Subtle swelling around the lips and lower face slowly resolves over this period — what looks “final” at three months is often even better at six. Sensation continues to return. Final orthodontic adjustments happen during this window for many patients.
Months 6-12: the full result
Most patients see their final result somewhere between nine months and a year. Bone is fully healed, sensation is largely back (subtle areas of altered sensation can persist), and any orthodontic refinement is complete. Long-term outcomes — including airway, joint health, and bite stability — are tracked through routine follow-up.
What about TMJ replacement and revision cases?
Recovery from total TMJ replacement or complex orthognathic revision surgery is generally a few weeks longer at each stage compared to primary single-jaw surgery, mostly because the operations are bigger and physical therapy plays a more central role. The week-by-week pattern is similar; the curve is just shifted.
Things that slow recovery — and how to avoid them
- Tobacco and nicotine. Including vaping. Nicotine is a vasoconstrictor and slows bone healing significantly.
- Skipping protein. Healing requires protein. Patients on liquid diets need to plan for it deliberately.
- Skipping physical therapy. Especially after joint surgery.
- Returning to chewing too early. Bone consolidation takes weeks. Premature chewing causes problems.
- Sleeping flat. Elevation reduces swelling and is recommended for the first 1-2 weeks.
The postoperative instructions page has more detailed guidance.
What about pain?
This is the part patients are most surprised by. Modern jaw surgery hurts much less than people expect. Most patients describe the dominant sensation as pressure, congestion, and tightness rather than sharp pain. Long courses of opioid pain medication are usually not needed. Effective pain control plans typically combine scheduled non-opioid medications with short, limited use of stronger medications only when needed. Information from the CDC and other public health sources reinforces the importance of minimizing opioid exposure when possible.
The bottom line
Most jaw surgery patients are looking like themselves at three to four weeks, working at two to four weeks, exercising at six to eight weeks, eating normally at six to eight weeks, and at their final result somewhere between six and twelve months. It’s a long but very manageable process when you know what to expect.
To start a conversation about jaw surgery and what your specific recovery would look like, schedule a consultation or call 214.828.9115. Travel logistics for out-of-area patients are addressed on the travel information page.