If you’ve ever taken a bite of a sandwich and heard a click loud enough that the person across the table looked up, you’re not alone. Jaw clicking, popping, grinding, and crunching are some of the most common reasons people start searching for answers about their temporomandibular joint, or TMJ.
Most of the time the question patients really want answered is simple: is this normal, or is something wrong? The honest answer is that it depends on what kind of sound you’re hearing, what else is happening, and how long it has been going on.
What is the TMJ, and why does it make noise?
The temporomandibular joint is the joint in front of each ear that connects your lower jaw to your skull. It’s one of the most complex joints in the body because it doesn’t just hinge open and closed — it also slides forward and side to side every time you talk, chew, or yawn.
Inside the joint sits a small fibrocartilaginous disc that acts as a cushion between the jawbone and the skull. When that disc is in the right position, the joint moves silently. When it slips out of place, gets damaged, or starts to break down, the joint can produce sounds. You can read more about the anatomy and pathology of the joint on the TMJ Dysfunction overview page. The U.S. National Institute of Dental and Craniofacial Research also has helpful background on TMJ disorders for general readers.
The four most common TMJ sounds and what they usually mean
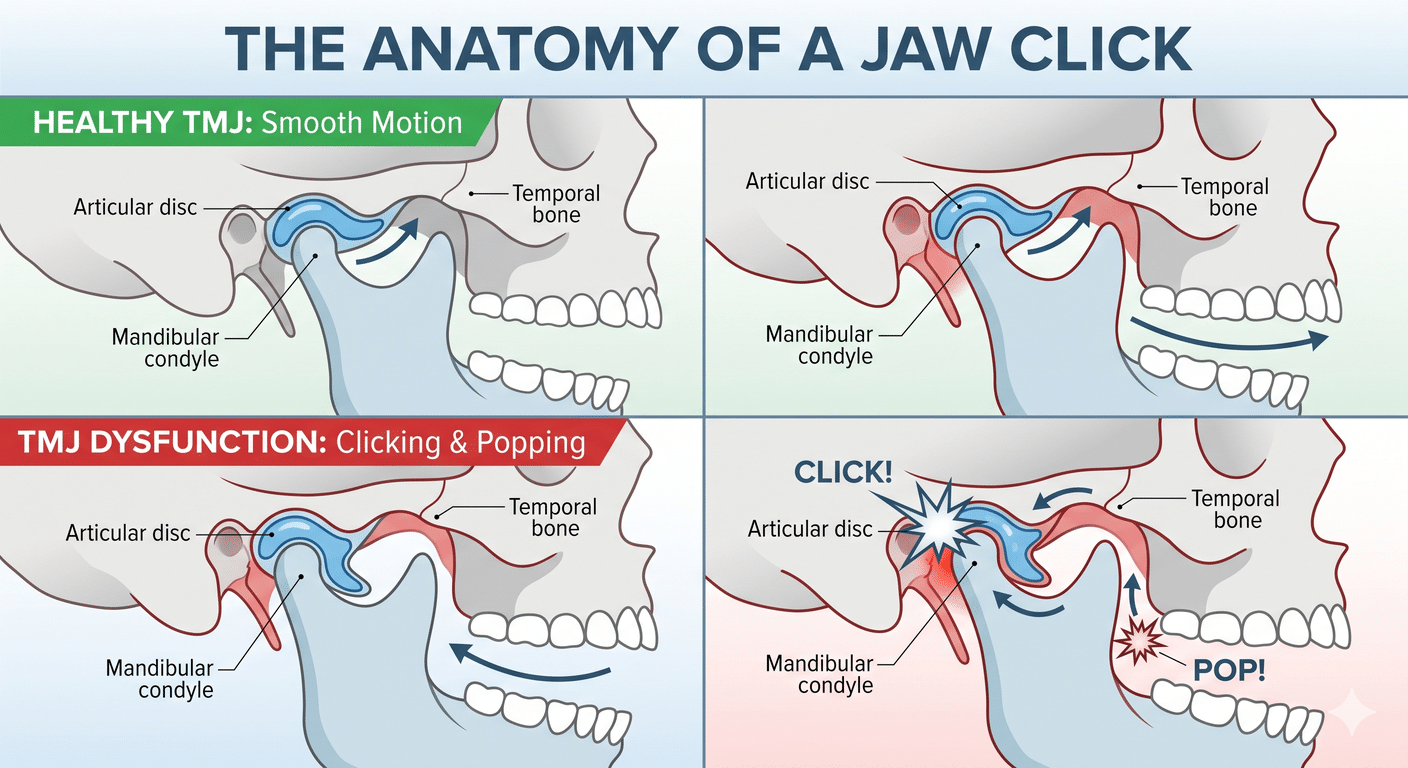
1. Clicking or popping
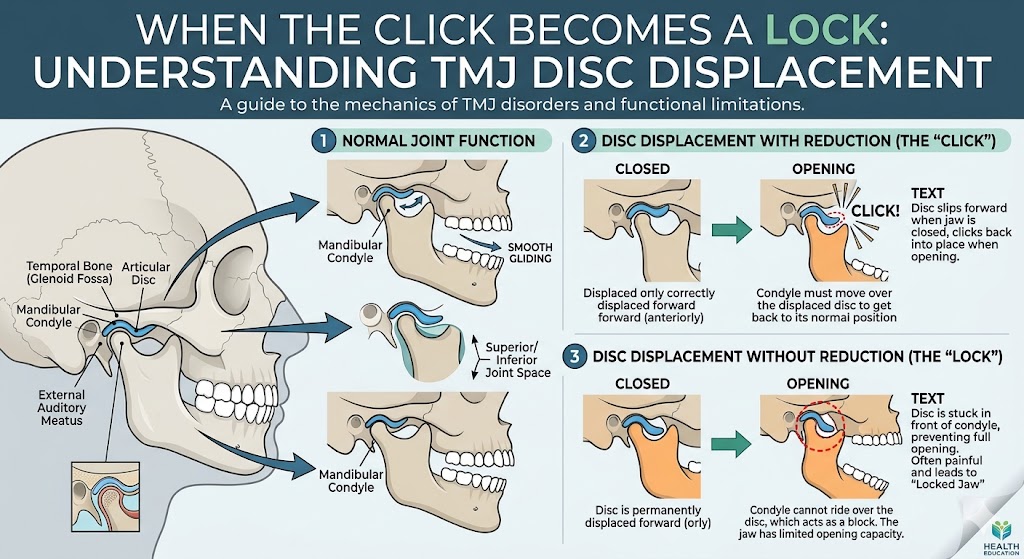
A single click when you open or close your mouth is often a sign that the disc inside the joint is displaced. The disc slides out of position and then snaps back into place — that snap is the click you hear. This is called disc displacement with reduction, and many people live with it for years without significant symptoms.
It becomes a bigger concern when the click gets louder, becomes painful, or is joined by limited opening. That can mean the disc is starting to get stuck out of place permanently.
2. Grinding or grating (crepitus)
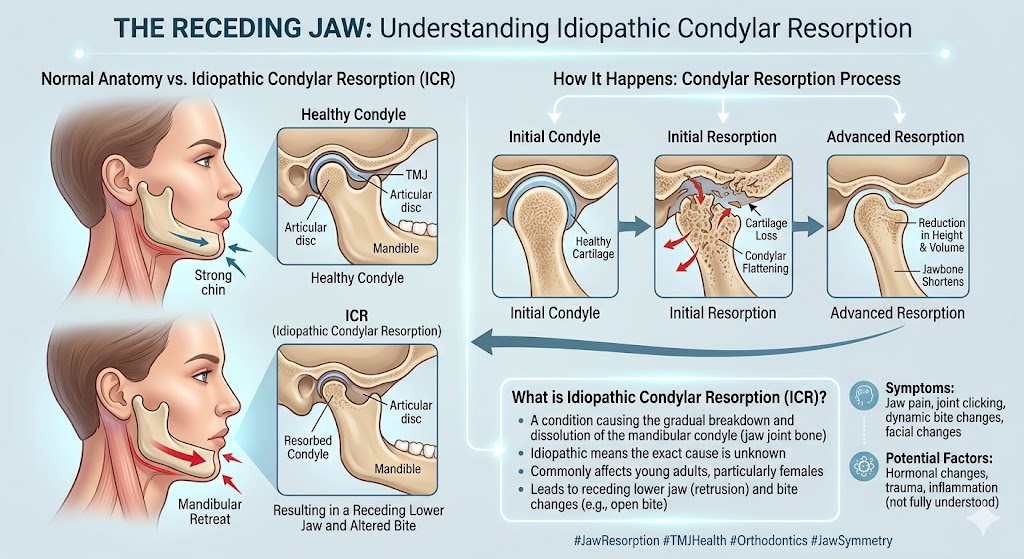
A grinding, sandy, or crunching sound is different. That sound usually means the smooth surfaces of the joint have started to wear down — essentially arthritis inside the TMJ. It’s often a sign of more advanced joint disease, including conditions like mandibular condylar resorption or osteoarthritis of the joint. The Arthritis Foundation has additional patient-friendly information on how arthritis affects joints throughout the body.
3. Locking, with or without sound
If your jaw locks open or locks closed, even briefly, that is not something to ignore. It typically means the disc is no longer reducing — it’s stuck. Closed lock often presents as the inability to open more than about 25 to 30 millimeters (roughly two finger-widths). Open lock means you can’t close your mouth back down. Either is a reason to be evaluated promptly.
4. Sudden silence after years of clicking
This one surprises people. Many patients are relieved when a long-standing click suddenly disappears. But sometimes the silence means the disc is now permanently displaced and can no longer relocate at all. If your click vanished and you also lost some range of motion, that change deserves attention.
When jaw clicking is not an emergency
A painless click that has been there for years, doesn’t limit your opening, and doesn’t get worse is usually not dangerous on its own. Many people have a low-grade click for life and never need surgery. The goal in those cases is to monitor and avoid making it worse — that means avoiding gum chewing, ice crunching, very chewy foods, wide yawning, and clenching.
When jaw sounds become a red flag
It’s time to see a specialist when any of the following are true:
- Your clicking is now painful, not just noisy.
- You can no longer open your mouth wide enough to bite a sandwich.
- Your bite has changed — your teeth don’t meet the way they used to.
- You’re getting headaches, ear pain, or facial pain along with the sounds.
- Your jaw locks, even occasionally.
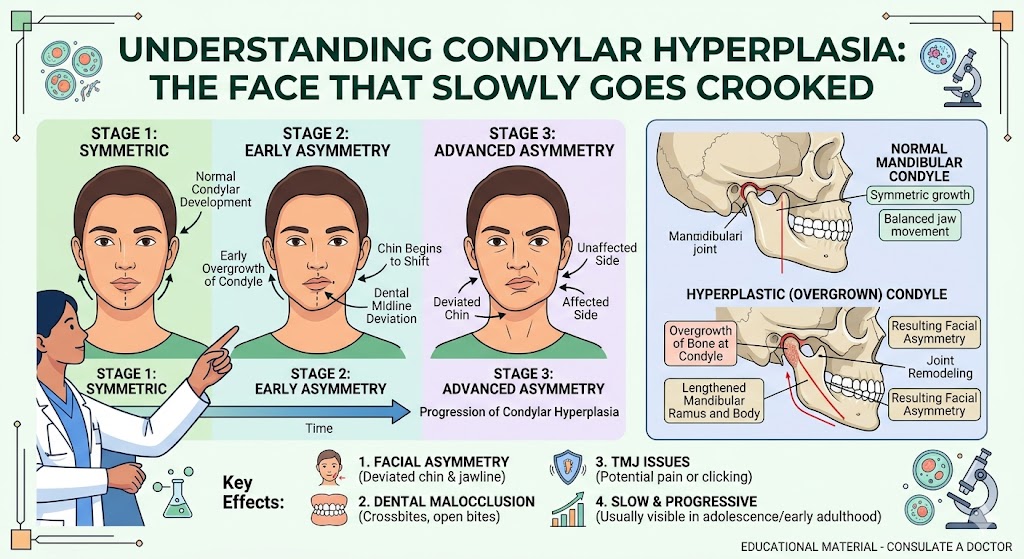
- Your chin or face looks asymmetric or seems to be receding.
Bite changes especially are an important sign. When the bite shifts on its own, something structural is changing inside the joint. That’s a common pattern in adolescent internal condylar resorption and in TMJ reactive arthritis, both of which can quietly destroy the joint if missed.
How a TMJ specialist actually evaluates joint sounds
A real evaluation goes well beyond listening to your jaw. The workup typically includes a detailed medical history, a clinical exam of the joint and bite, and imaging — most importantly an MRI of the TMJ to see the disc and surrounding tissues, plus a CT or cone-beam CT to evaluate the bone. Many patients benefit from a comprehensive diagnosis and treatment planning consultation before any treatment decisions are made.
Patients can begin the process by completing the TMJ pain questionnaire, which helps gather the right information before the evaluation.
What treatment looks like (and why surgery is rarely the first step)
Most TMJ patients never need surgery. Conservative care — soft diet, anti-inflammatory medication, physical therapy, occlusal splints, and stress management — resolves a large percentage of joint clicking and pain. Surgery comes into the picture only when the joint is structurally damaged, when there’s progressive bite change, or when conservative care has failed.
When surgery is needed, the spectrum runs from minimally invasive arthroscopy and arthroplasty up to total TMJ replacement for end-stage disease. Many cases also require concurrent complex orthognathic revision surgery to correct the bite and facial structure that the joint disease has changed.
The bottom line
Jaw clicking and popping is extremely common and often not serious. But sound plus pain, sound plus limited opening, sound plus a changing bite, or sudden locking are all signals that something inside the joint is changing. Catching that early matters — many TMJ disorders are far easier to manage before they become end-stage.If your jaw is making noises that worry you, you can call 214.828.9115 for a free 15-minute telephone consultation, or schedule an evaluation with Dr. Wolford’s Dallas office.