Sleep apnea is a very common sleep disorder that can affect every facet of a patient’s life. In addition to sleep deprivation and its many effects, this sleep disorder may also affect heart health and mental health. Dr. Larry Wolford, Clinical Professor of Oral and Maxillofacial Surgery, offers sleep apnea treatment to help patients reclaim their quality of life.
What Is Sleep Apnea and How Does It Affect Health?
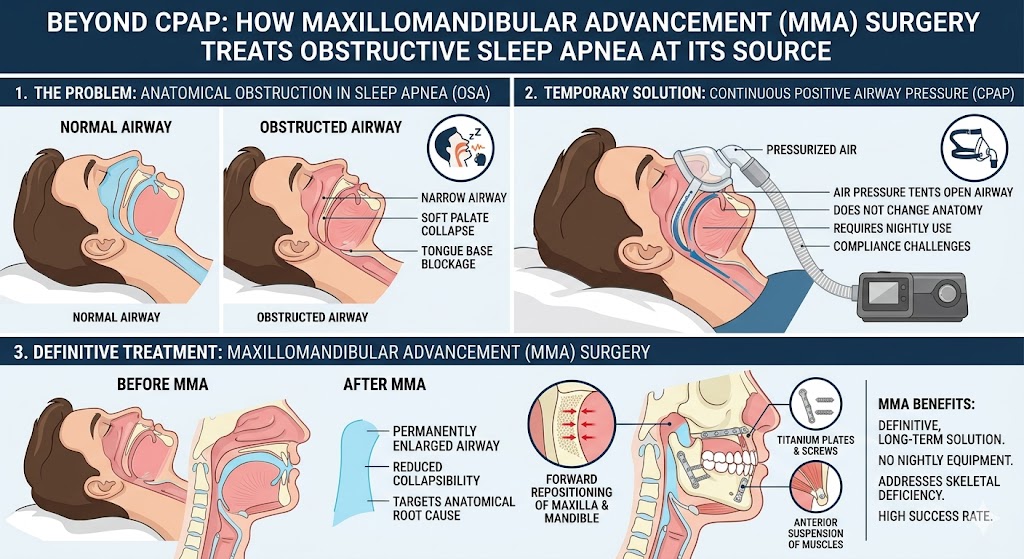
Sleep apnea is a condition that impedes a patient from breathing properly during sleep. This occurs because soft tissues in the mouth collapse during sleep and ultimately block air passageways. When the patient stops breathing, the body wakes to reinitiate proper breathing. Throughout the night, a sleeper can cease breathing and wake hundreds of times.
This sleep disorder prevents a patient from progressing through the various stages of sleep and instead robs them of the ability to gain rejuvenating rest. Patients will wake in the morning with headaches, dry mouth, and noticeable fatigue—even if they thought they slept a full eight hours.
Without sleep apnea treatment, patients will eventually suffer from the effects of severe sleep deprivation, including memory loss, depression, chronic fatigue, and unhealthy oxygen levels. Many researchers have learned that sleep apnea may affect cardiovascular health, too. This is due to the sleeper’s inability to maintain a steady, lowered heart rate during sleep. The cycle of apnea and wakefulness may weaken the heart over time.
What Are Some Common Methods for Sleep Apnea Treatment?
The treatment indicated for obstructive sleep apnea varies based on the needs of each patient. The symptoms of sleep apnea may be improved with treatment such as the use of oral appliances to re-position the lower jaw and changes in lifestyle that include cessation from tobacco and weight loss. Other patients may require oral surgery to fix nasal obstructions, jaw misalignment, or enlarged soft oral tissues. Our oral surgeon will determine the underlying cause(s) of sleep apnea to develop the best treatment possible.
If you have questions or would like to schedule an appointment, please contact Dr. Larry Wolford’s office using our online contact form or call 214-828-9115.