Temporomandibular Joint – TMJ Disorder Symptoms may include seemingly unexplained facial or jaw pain and/or pain that radiates into the neck and shoulders, headaches and earaches, and a locking of the jaw.
The jaw is a highly complex joint, composed of several different components that must work in concert for the joint to function properly and be capable of both lateral and vertical movements. Unfortunately, problems may develop in the temporomandibular joint (TMJ) that may cause painful symptoms.
Find Out TMJ Disorder Symptoms
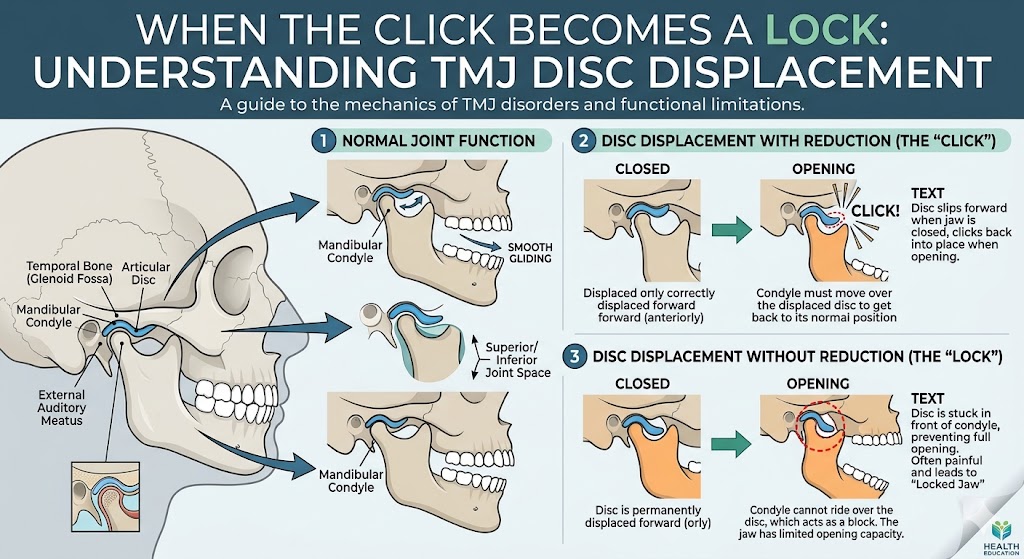
You or your oral surgeon may suspect that you have a TMJ disorder if you present with certain symptoms. A clicking or popping sound while opening or closing the jaw is often a telltale sign. Other TMJ disorder symptoms may include seemingly unexplained facial or jaw pain and/or pain that radiates into the neck and shoulders, headaches and earaches, and a locking of the jaw.
Stress may also exacerbate a TMJ disorder that is already present.
Other, more subtle, indicators include changes in facial appearance, lightheadedness and a need to change the diet to favor softer foods.
Certain characteristics may make people more susceptible to TMJ disorders. For example, a malocclusion (“bad bite”) or other congenital jaw abnormality can contribute to pain in the joint. Stress may also exacerbate a TMJ disorder that is already present.
If you complain of TMJ disorder symptoms that are potentially caused by TMJ, your oral surgeon will complete a thorough evaluation of your case. You likely will need to have x-rays taken so that your surgeon will have a birds-eye view of the jaw joint. This perspective will help the oral surgeon diagnose the specific nature of the problem and plan for treatment.
TMJ Disorders Causes
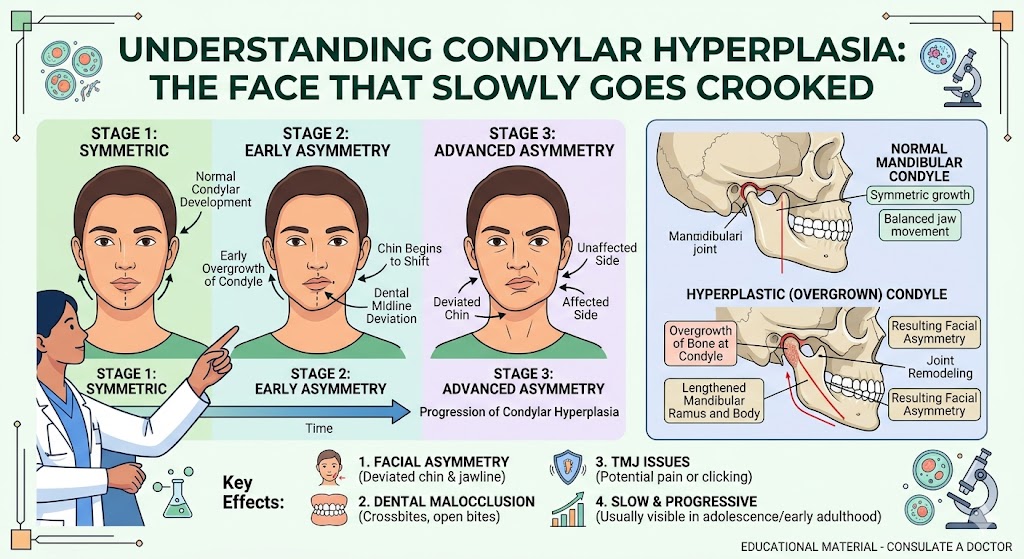
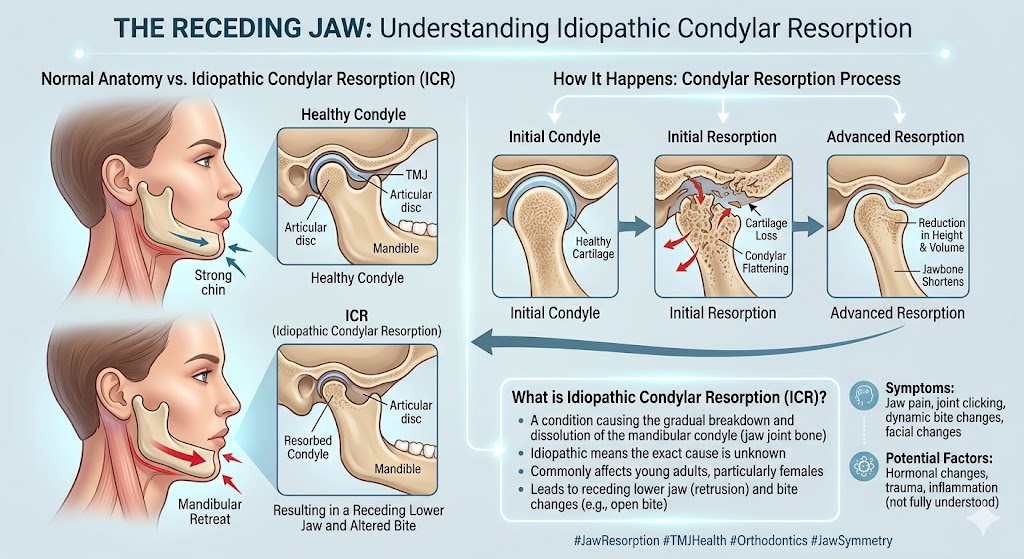
TMJ disorders often may result from problems with the disc or improper growth patterns of the jaw during puberty. As a result, early intervention during the teen years may be able to minimize a patient’s chances of having TMJ disorders later in life.
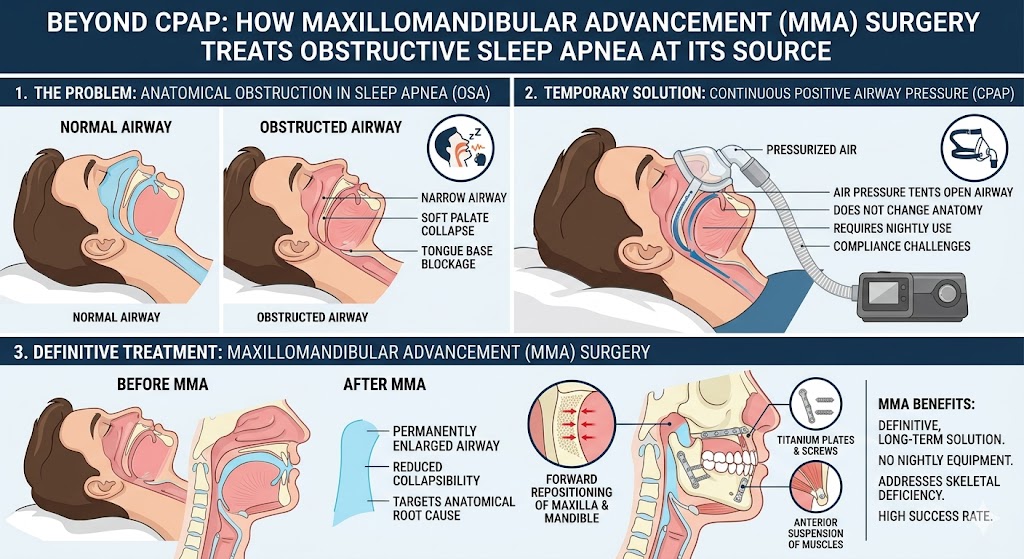
Older patients with TMJ issues may benefit from surgical interventions to reposition the jaw or correct the problematic structure causing the discomfort. Patients who develop TMJ due to autoimmune conditions, like rheumatoid arthritis or lupus, may need to be fitted with a prosthetic joint in order to get relief from their symptoms.
Don’t feel that you have to suffer from TMJ disorder symptoms associated with TMJ disorders. You can discuss your treatment options with our experienced oral and maxillofacial surgery team.
If you have questions or would like to schedule an appointment, please contact Dr. Larry Wolford’s office using our online contact form or call 214-828-9115.