There is no doubt about it: breathing is essential to life. The simple act of inhaling and exhaling fills our bodies with oxygen. Our brains and muscles cannot function without it, and both mentally and physically, a lack of oxygen can have disastrous effects.
Sleep Apnea
During the day, breathing happens so easily that we rarely think about it at all. But, what happens at night, as you sleep, when the act of breathing isn’t so easy? Millions of adults suffer from a condition known as sleep apnea, in which breathing while sleeping is a challenge.
Sometimes, the condition is caused by improper brain function. Whereas the brain would normally prompt the body to inhale and exhale, a patient with sleep apnea may not receive those brain signals. The result is a failure to breathe regularly, and the lack of oxygen can create a major health risk.
Obstructive Sleep Apnea
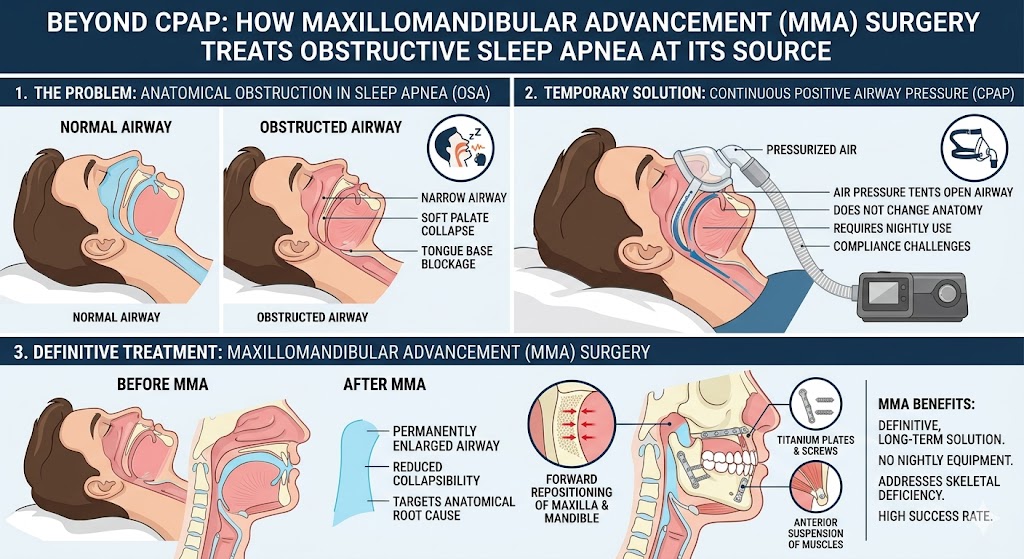
More often, the brain is able to send the appropriate breathing signals, but the airways of the nose, mouth, or throat is blocked, hindering the process. The blockage can be the result of the tongue or soft palate relaxing across the opening of the throat. It can be exacerbated by obesity or constricted nasal passages. This form of apnea, called obstructive sleep apnea, is more common and can render the same unhealthy results.
Both forms of sleep apnea tend to occur frequently throughout the night, harming your organs and interrupting your sleep pattern.
Imagine how your quality of life, energy, and mental stamina would be affected by a lack of oxygen and a lack of sleep. You’d probably snore quite loudly, feel groggy and tired during the day, feel irritable, and find it challenging to concentrate. Severe cases can lead to depression, weight gain, and car accidents or workplace injuries.
Fortunately, your oral surgeon can help treat various sleep apnea levels using surgical and non-surgical methods. It’s the right choice for your mental and physical health.
If you have questions or would like to schedule an appointment, please contact Dr. Larry Wolford’s office using our online contact form or call 214.828.9115.