If you’ve been struggling with jaw misalignment or facial irregularities, you may have heard of orthognathic surgery as a potential solution. But how do you know if you’re a suitable candidate for this transformative procedure? Look no further, as we delve into the key factors that determine your eligibility for orthognathic surgery. In this comprehensive guide, we’ll explore the various conditions that may warrant orthognathic surgery, such as severe overbites, underbites, and crossbites. We’ll also discuss the potential benefits and risks associated with this surgical intervention, along with the recovery process and expected outcomes. Whether you’re seeking to improve your appearance, alleviate pain, or enhance your overall oral health, understanding the candidacy criteria for orthognathic surgery is crucial. So, if you’re curious to find out if you’re a suitable candidate for this life-changing procedure, keep reading to uncover the answers you’ve been looking for.
What is Orthognathic Surgery?
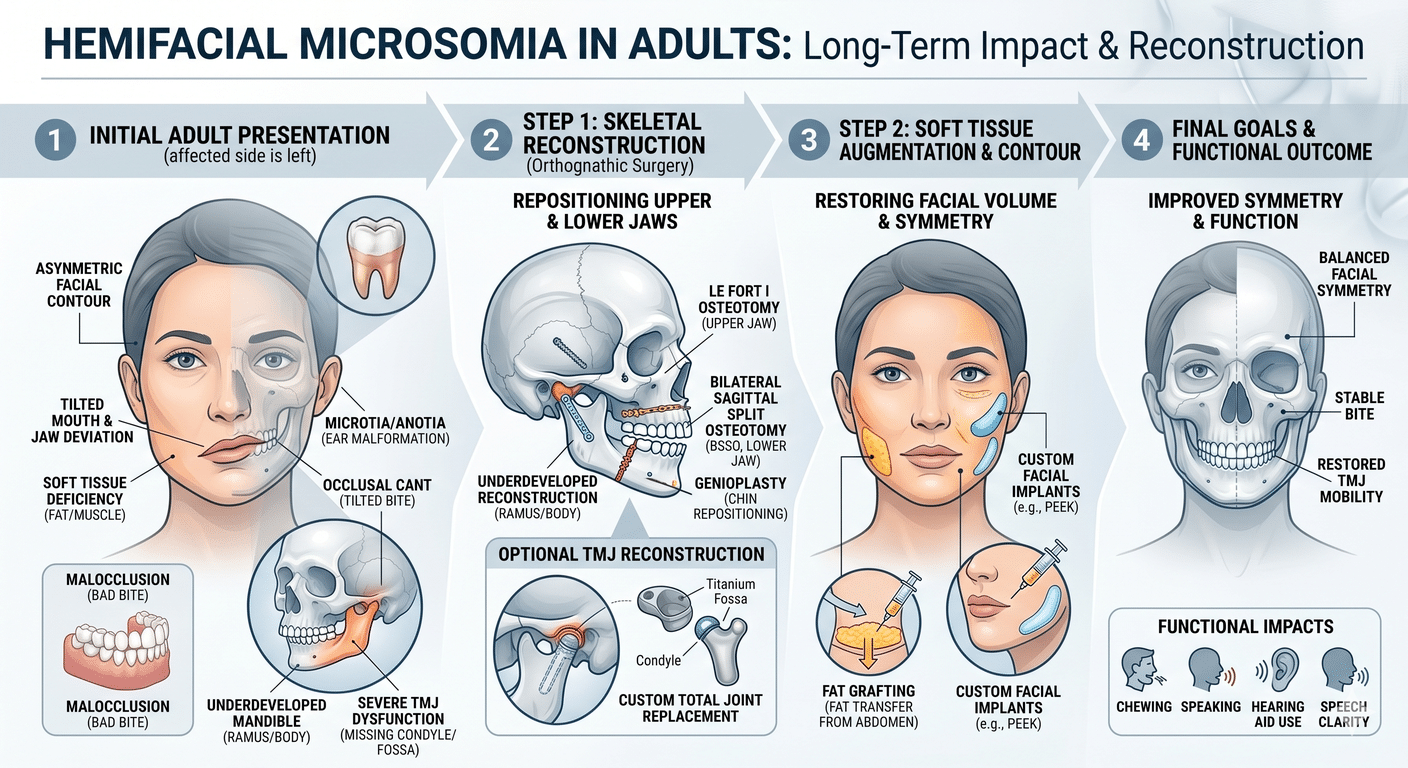
Orthognathic surgery, also known as corrective jaw surgery, is a type of surgical intervention that aims to correct jaw misalignment and facial irregularities. It involves repositioning the upper jaw (maxilla), lower jaw (mandible), or both to achieve proper alignment and improve the functionality and aesthetics of the face. This procedure is typically performed by an oral and maxillofacial surgeon in collaboration with an orthodontist, as braces are often used in conjunction with orthognathic surgery to ensure optimal results.
Orthognathic surgery is a complex procedure that requires careful planning and precise execution. It is usually recommended for individuals who experience severe jaw misalignment that cannot be adequately addressed through orthodontic treatment alone. By addressing the underlying structural issues, orthognathic surgery can improve a wide range of conditions, including severe overbites, underbites, crossbites, open bites, and facial asymmetry.
Signs that You May be a Candidate for Orthognathic Surgery
Determining whether you’re a suitable candidate for orthognathic surgery involves a thorough evaluation of various factors. Some signs that may indicate the need for this procedure include:
1. **Severe Jaw Misalignment:** If you have a significant discrepancy between your upper and lower jaws, resulting in functional problems such as difficulty chewing or speaking, orthognathic surgery may be recommended.
2. **Aesthetic Concerns:** Orthognathic surgery can also address cosmetic issues related to jaw misalignment, such as a protruding or recessed jawline, an imbalanced facial appearance, or a “gummy” smile.
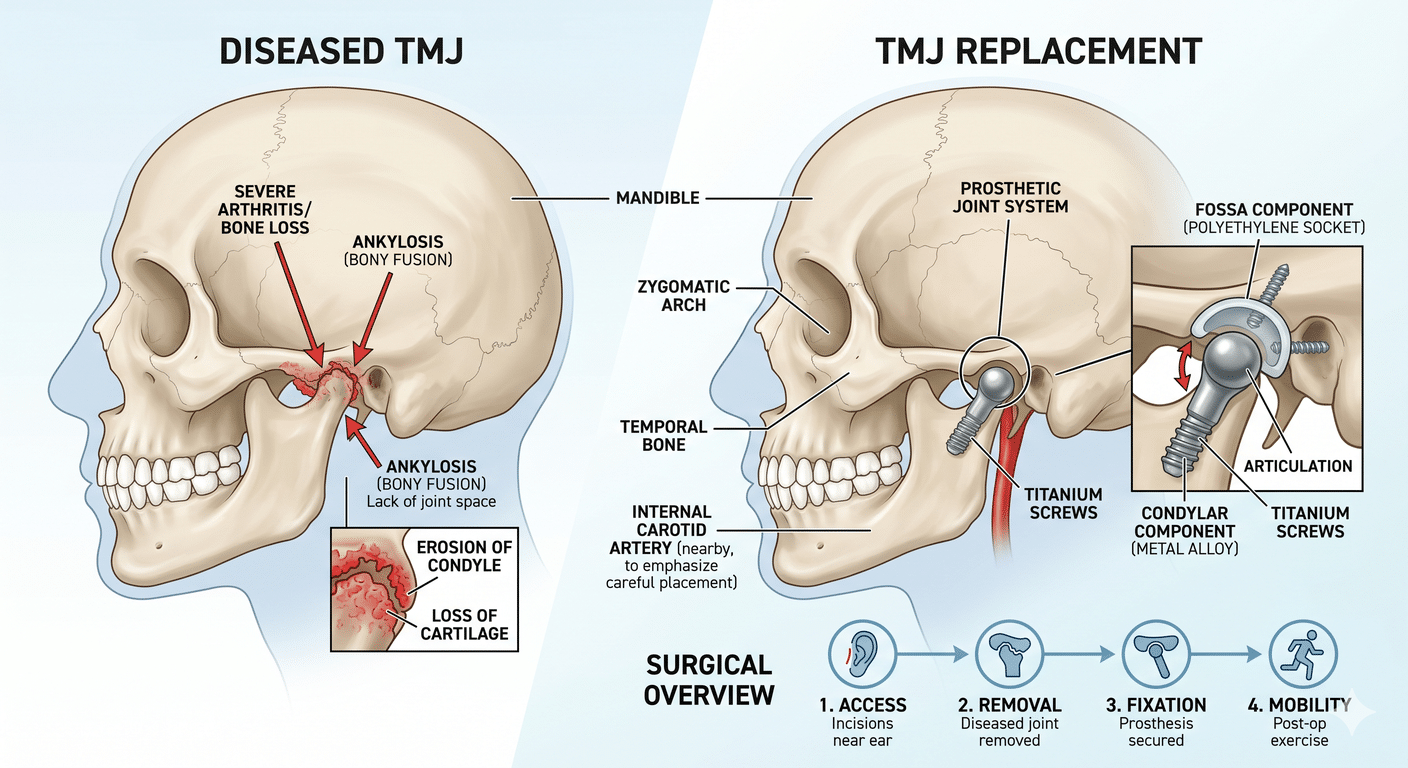
3. **Chronic Jaw Pain:** If you experience chronic jaw pain, temporomandibular joint (TMJ) disorders, or headaches that are caused by jaw misalignment, orthognathic surgery may provide relief.
4. **Breathing Problems:** In some cases, orthognathic surgery may be necessary to correct airway obstructions caused by a narrow upper jaw or other structural abnormalities. This can improve breathing and alleviate symptoms of sleep apnea.
5. **Problems with Oral Health:** Orthognathic surgery can also help address oral health issues such as difficulty maintaining proper oral hygiene due to crowded teeth, recurring dental problems, or excessive wear on the teeth.
If you experience any of these signs, it’s essential to consult with an oral and maxillofacial surgeon who specializes in orthognathic surgery. They will evaluate your specific condition and determine whether you’re a suitable candidate for this procedure.
Benefits of Orthognathic Surgery
Orthognathic surgery offers a range of benefits that go beyond cosmetic improvements. Some of the key advantages of this procedure include:
1. **Improved Facial Aesthetics:** By repositioning the jaws, orthognathic surgery can enhance the overall balance and symmetry of the face, resulting in a more pleasing appearance.
2. **Enhanced Oral Functionality:** Orthognathic surgery can improve chewing, speaking, and swallowing functions by aligning the jaws properly. This can have a positive impact on your overall quality of life.
3. **Alleviation of Pain:** If you experience chronic jaw pain or headaches caused by jaw misalignment, orthognathic surgery can provide significant pain relief and improve your daily comfort.
4. **Better Oral Health:** By addressing structural issues that contribute to dental problems, orthognathic surgery can make it easier to maintain proper oral hygiene and reduce the risk of tooth decay, gum disease, and other oral health issues.
5. **Improved Breathing:** For individuals with airway obstructions or sleep apnea, orthognathic surgery can help open up the airway, making it easier to breathe and improving the quality of sleep.
It’s important to note that the benefits of orthognathic surgery may vary depending on the specific condition being addressed and the individual’s unique circumstances. It’s crucial to consult with a qualified oral and maxillofacial surgeon to understand how orthognathic surgery can benefit you personally.
The Orthognathic Surgery Process
Orthognathic surgery is a multi-step process that involves careful planning, preparation, and collaboration between the oral and maxillofacial surgeon and orthodontist. Here’s an overview of the typical orthognathic surgery process:
1. **Initial Consultation:** The process begins with an initial consultation with an oral and maxillofacial surgeon. During this appointment, the surgeon will evaluate your condition, discuss your treatment goals, and explain the surgical options available to you.
2. **Orthodontic Treatment:** In most cases, orthodontic treatment is an essential part of the orthognathic surgery process. Before surgery, you may need to wear braces to align your teeth properly and prepare them for the surgical procedure.
3. **Surgical Planning:** Once your teeth are properly aligned, the oral and maxillofacial surgeon will develop a comprehensive surgical plan. This plan will take into account your specific condition, treatment goals, and any functional or aesthetic concerns.
4. **Surgical Procedure:** The actual surgery is typically performed under general anesthesia in a hospital or surgical center. The surgeon will make incisions inside the mouth to access the jawbone and reposition it as planned. In some cases, additional surgical techniques may be used, such as genioplasty (chin surgery) or bone grafting.
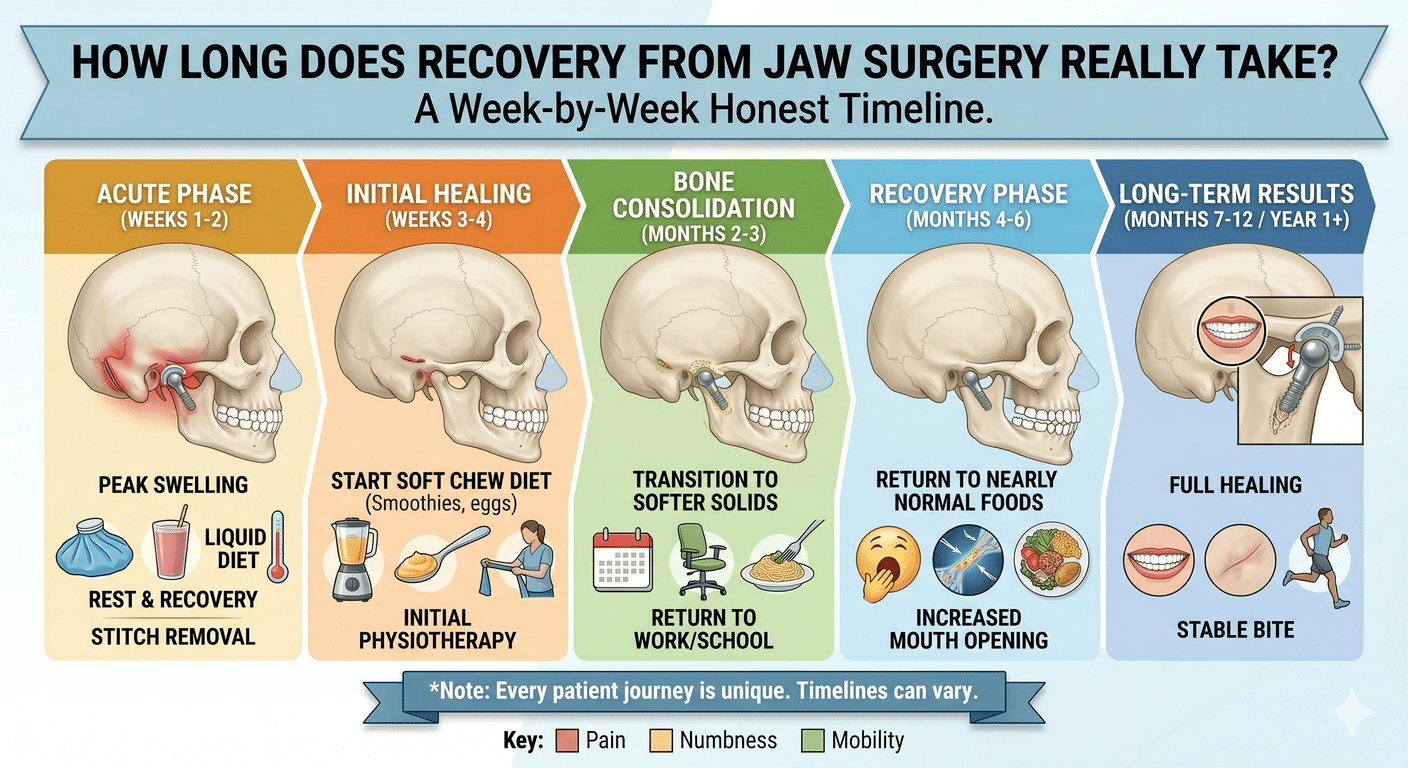
5. **Recovery and Rehabilitation:** After the surgery, you will be closely monitored in a recovery area until you wake up from the anesthesia. You can expect some swelling, discomfort, and bruising in the days following the surgery. Your surgeon will provide you with specific post-operative instructions, including dietary restrictions, pain management techniques, and oral hygiene guidelines.
6. **Orthodontic Follow-up:** Following the surgery, you will continue your orthodontic treatment to fine-tune your bite and ensure optimal alignment. This phase may involve adjustments to your braces, wearing elastics, or using other orthodontic appliances.
The duration of the orthognathic surgery process varies depending on the complexity of the case and the individual’s healing rate. It’s important to follow all instructions provided by your surgical team and attend all necessary follow-up appointments to achieve the best possible outcomes.
Preparing for Orthognathic Surgery
Preparing for orthognathic surgery involves several important steps to ensure a smooth and successful procedure. Here are some key considerations:
1. **Consultation and Evaluation:** Schedule an initial consultation with an oral and maxillofacial surgeon who specializes in orthognathic surgery. During this appointment, the surgeon will evaluate your condition, discuss your treatment goals, and explain the surgical process in detail.
2. **Orthodontic Treatment:** In most cases, orthodontic treatment is necessary before orthognathic surgery. This phase aims to align your teeth properly and create a stable foundation for the surgical procedure. It may involve wearing braces or other orthodontic appliances for a specific period.
3. **Medical Evaluation:** Your surgical team will typically request a comprehensive medical evaluation to ensure your overall health and fitness for surgery. This may include blood tests, imaging studies, and consultations with other specialists if necessary.
4. **Psychological Preparation:** Orthognathic surgery is a significant procedure that can have a profound impact on your appearance and overall well-being. It’s important to prepare yourself mentally and emotionally for the changes that will occur. If needed, consider seeking support from a therapist or counselor to help you navigate any concerns or anxieties.
5. **Financial Considerations:** Orthognathic surgery can be a substantial financial investment. It’s essential to discuss the cost of the procedure, including any related expenses such as orthodontic treatment, with your surgical team and insurance provider. Explore available payment options and determine the most suitable financial plan for your situation.
By taking these steps and working closely with your surgical team, you can ensure that you’re fully prepared for the orthognathic surgery process.
What to Expect During and After Orthognathic Surgery
During orthognathic surgery, you will be placed under general anesthesia to ensure your comfort and safety throughout the procedure. The surgery itself typically takes several hours, depending on the complexity of your case. The oral and maxillofacial surgeon will make incisions inside your mouth to access the jawbone and perform the necessary adjustments. In some cases, additional incisions may be made externally, but this is less common.
After the surgery, you will be moved to a recovery area where you will wake up from the anesthesia. You can expect some swelling, discomfort, and bruising in the days following the procedure. Your surgeon will provide you with detailed post-operative instructions, including pain management techniques, dietary restrictions, and oral hygiene guidelines. It’s important to follow these instructions closely to ensure proper healing and minimize the risk of complications.
During the recovery period, you will need to rest and avoid strenuous activities. Your surgeon may prescribe pain medication to manage any discomfort, and you should attend all follow-up appointments as scheduled. It’s crucial to maintain good oral hygiene by gently brushing your teeth and rinsing your mouth with a prescribed mouthwash. You may also need to follow a soft or liquid diet for a certain period to allow your jaws to heal properly.
The initial swelling and discomfort will gradually subside over the following weeks, and you should start to notice improvements in your facial appearance and oral functionality. However, it’s important to note that the complete healing process can take several months, and the final results may not be fully evident until then.
Recovery and Rehabilitation After Orthognathic Surgery
Recovery and rehabilitation after orthognathic surgery are crucial for achieving the best possible outcomes. Here are some important aspects to consider during the recovery period:
1. **Managing Discomfort:** You can expect some swelling, discomfort, and bruising in the days following the surgery. Your surgeon will prescribe pain medication to help manage any discomfort. It’s important to take the medication as directed and avoid any over-the-counter pain relievers without your surgeon’s approval.
2. **Dietary Considerations:** Your surgeon will provide you with specific dietary instructions to follow during the initial stages of recovery. This may involve consuming a soft or liquid diet to allow your jaws to heal properly. It’s important to stick to these guidelines to avoid any complications or delays in the healing process.
3. **Oral Hygiene:** Maintaining good oral hygiene is crucial during the recovery period. Your surgeon will provide you with instructions on how to brush your teeth gently and rinse your mouth with a prescribed mouthwash. It’s important to follow these guidelines to prevent infections and promote proper healing.
4. **Physical Activity:** It’s important to avoid strenuous physical activities and exercise during the initial stages of recovery. Your surgeon will provide you with specific guidelines on when it’s safe to resume normal activities. It’s important to follow these guidelines to prevent any complications or delays in the healing process.
5. **Follow-up Appointments:** Regular follow-up appointments with your surgical team are essential for monitoring your progress and ensuring proper healing. It’s important to attend all scheduled appointments and raise any concerns or questions you may have during these visits.
During the recovery period, it’s normal to experience some ups and downs in your physical and emotional well-being. It’s crucial to be patient with the healing process and reach out to your surgical team if you have any concerns or questions.
Risks and Complications of Orthognathic Surgery
Like any surgical procedure, orthognathic surgery carries some risks and potential complications. It’s important to be aware of these before making a decision. While complications are relatively rare, they can include:
1. **Infection:** Infection is a potential risk associated with any surgical procedure. Your surgical team will take precautions to minimize this risk, and it’s important to follow all post-operative care instructions to reduce the likelihood of infection.
2. **Bleeding:** Some bleeding is expected during and immediately after surgery. However, excessive bleeding can occur in rare cases. Your surgical team will monitor your condition closely to ensure proper hemostasis.
3. **Nerve Damage:** There is a small risk of temporary or permanent nerve damage during orthognathic surgery. This can result in altered sensation, numbness, or tingling in the face, lips, or tongue. However, the risk of significant nerve damage is relatively low in experienced hands.
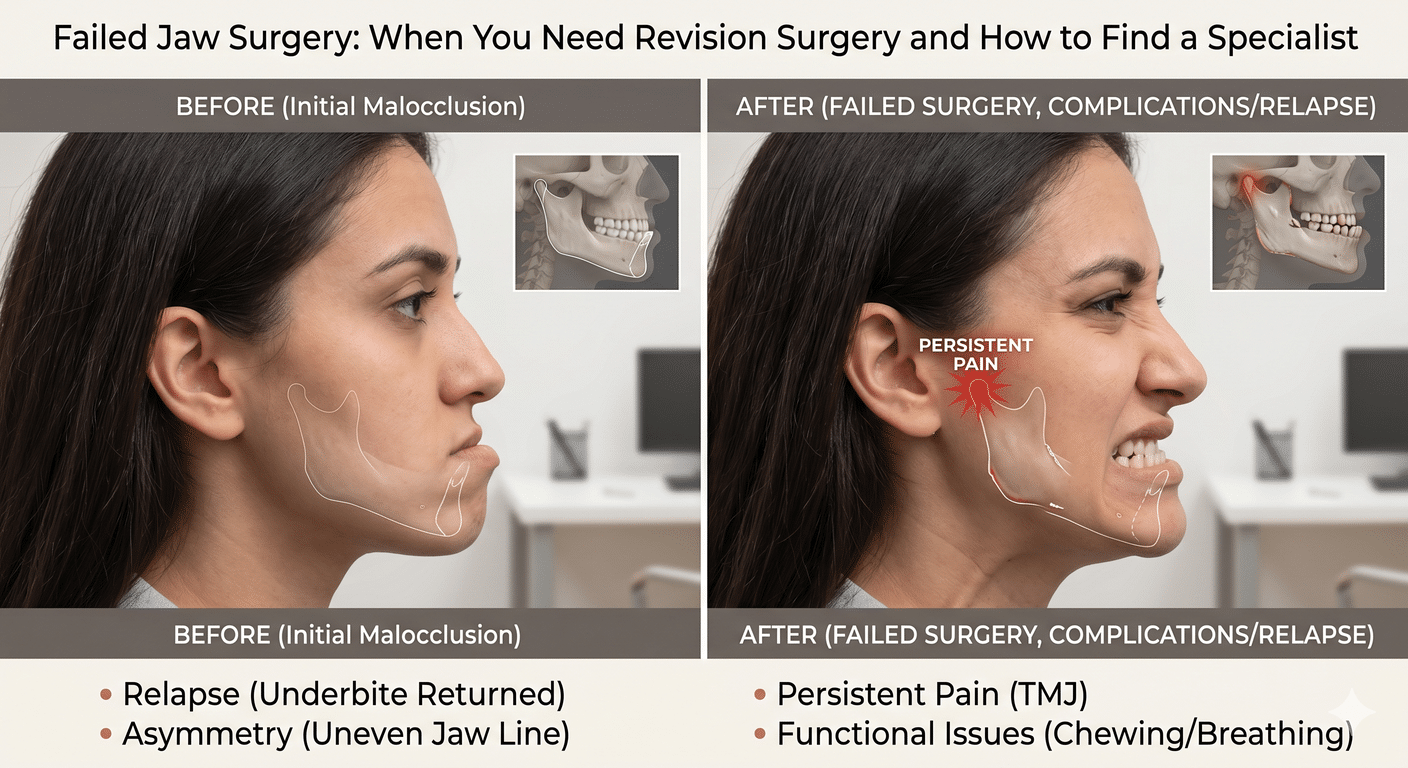
4. **Malocclusion:** In some cases, the final alignment of the jaws may not be optimal, resulting in a less than ideal bite. This can be addressed through additional orthodontic treatment or, in rare cases, a revision surgery.
5. **Relapse:** Over time, there is a potential for relapse, especially if post-operative instructions and orthodontic treatment are not followed diligently. Regular follow-up appointments and ongoing orthodontic care are essential to maintain the results achieved through orthognathic surgery.
It’s important to discuss any concerns or questions you may have about the potential risks and complications with your surgical team. They will provide you with detailed information and address any specific concerns related to your case.
Alternative Treatments to Orthognathic Surgery
While orthognathic surgery is a highly effective treatment for jaw misalignment and facial irregularities, it’s not the only option available. Depending on your specific condition and treatment goals, your surgical team may recommend alternative treatments. Some common alternatives to orthognathic surgery include:
1. **Orthodontic Treatment Only:** In some cases, mild to moderate jaw misalignment can be addressed through orthodontic treatment alone. This may involve wearing braces or other orthodontic appliances to